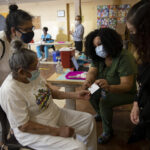
Victoria Roberts, vice president of health services for D.C. non-profit Community of Hope, says vaccine rollout has been a bit of a trial and error system since D.C.’s Department of Health first made doses available for residents 65 and older in mid-January.
Community of Hope primarily provides D.C.’s low-income communities, mostly Black and Latino residents, with housing and healthcare services — but when the DC Health portal went live, that’s not who showed up at the organization’s clinics.
“The people who were coming in were not representative of our typical patients, and our patients were not able to get those appointments,” Roberts says.
Not only were there technical glitches in the system, but Roberts says her staff noticed a few names of notable D.C. public figures on the appointments list — people who had never scheduled appointments at the organization’s clinics before.
“I was frustrated to find that there were people whose names I recognized. They’re well-known people in D.C. who, I don’t know how they managed to game the system,” she says. “They must have had multiple appointments because they no-showed for the appointments they made for us.”
African Americans make up less than half of the city’s population, but make up 74% of residents who have died from COVID-19. And almost immediately, it became clear that Black Washingtonians weren’t getting equitable access to vaccination appointments, despite the portal being available citywide. Appointments were filled within the first few hours, and residents in the wealthier Ward 3 managed to grab nearly 2,500 out of roughly 6,700 available spots (compared to 197 and 94 appointments in Ward 7 and Ward 8, respectively).
The D.C. Council — hearing reports of seniors waiting hours in long lines and lack of access for Black and Latino residents — pressured DC Health to open additional appointment slots for “priority zip codes” in Ward 1, 4, 5, 7, and 8.
Roberts says that after reporting Community of Hope’s scheduling issues to the health department, the staff was given permission to start scheduling appointments on their own, prioritizing their regular patients and seniors who were most at risk.
Things got off to a slow start — it took 250 calls to schedule just 40 appointments the first week, Roberts says — but the process has smoothed out over time. About 40% of the patients they reached signed up right away, another 40% were a “maybe,” and about 10 to 15% were a hard “no.” For those on the fence, Roberts says staff have been trained to answer any questions people might have about the vaccine safety and availability.
With the new system, Roberts says, Community of Hope is serving a group much more representative of its patient population. Other local clinics have had similar experiences.
Bread for the City CEO George Jones told The New York Times that when the portal opened, his community clinic was “full of white people.”
“We’d never had that before,” he said. “We serve people who are disproportionately African-American.”
Jones tells DCist that the statistics showing who was served before and after Bread for the City used the portal system were alarming. In the first week, only 22% of its available slots were taken by Black patients
“I really was floored when I walked into our clinic that first day and saw a room full of people in our waiting room—not because we have anything against white people, we certainly don’t,” Jones says. “But we’ve never had white patients, to be quite frank. It was a complete flip-flop of who you ordinarily would’ve seen in our clinic. And the more important piece, more than the optics, was, where were the people of color and their access to the vaccine?”
Once DC Health gave Bread for the City and other clinics the go ahead to take control of their own vaccine schedules, 73% of the appointments were filled by Black patients.
“What that signals to me is that if if you want to be equitable in any kind of public benefit or service in general, you have to you have to structure it so that it gets people of color who have been disadvantaged in so many indices in our society,” Jones says.
Mayor Muriel Bowser has repeatedly said most of these issues are tied to a scarcity of vaccine doses the federal government is producing and distributing. Clinic leaders echo those sentiments. Most can’t schedule appointments until the week ahead of time (or even the week of the appointments), when they’re told how many doses they’ll receive.
Elysia Jordan, director of clinical services at Mary’s Center, which primarily serves Latino populations across the area, says only one of their clinics is currently offering vaccines. The organization prioritizes its senior patients who are at a higher risk due to chronic diseases, but can’t reach all the people it wants to with its first allotment of 800 doses, she says.
“The biggest thing is supply,” says Jordan. ” We would need more supply to be able to do a higher volume of vaccinations. And ideally, we would want vaccines at all of our sites. There’s just not the supply for that right now.”
Even with the supply restraints, the District is working out its vaccination program, taking community feedback into consideration. D.C. now reserves 30% of its doses for residents who use the portal and the rest for programs like church clinics and community centers that serve people without access to reliable healthcare, transportation, or technology. (Howard University even launched a vaccine program to get more shots in arms.)
“This concept of taking vaccines to the people, we are actually doing that in the District of Columbia,” DC Health Director LaQuandra Nesbitt said at a recent press briefing, describing the groups that go door-to-door in underserved wards to offer appointments and information. Next month, District residents will be able to pre-register to be notified when they’re eligible to get vaccinated (although officials warn that it’s not a waitlist).
And the clinics, despite the initial hiccups, are working with what they’ve got, getting people vaccinated one patient at a time.
“Nothing’s been taken off our plate. Now, we’ve just added vaccination on top of it,” says Roberts, of Community of Hope. “But, you know, we’re getting experience. We’re learning. We’re always creative. We know how to duct tape pieces of things together to get the job done. That’s what we’ve always had to do. And so, we’re going to get this done.”
 Elliot C. Williams
Elliot C. Williams