Joyce Bumbray-Graves remembers her hands, dry and cracking from endless hours of handwashing.
“I had bandaids all over my fingers,” she says. “Oh my God, my hands were raw.”
The state of her hands is one of the few specifics that sticks out in her mind from a chaotic few weeks during the holidays. In one room of her house in Northern Virginia was her husband Andy, so sick with the coronavirus that he struggled to get out of bed. He communicated with her in whispers over a cell phone because the disease had stolen his breath.
Meanwhile, in another part of the house were Leia and Lisa, her adopted sister and her niece. Both are in wheelchairs— Leia has spina bifida and Lisa has cerebral palsy—and need round-the-clock care. Bumbray-Graves is a direct-to-consumer home health care worker, paid by Virginia’s state Medicaid program to feed, bathe, and care for Leia. Other home health care workers help with Lisa, but when Bumbray-Graves’ husband got sick with the coronavirus, she was on her own—taking care of him, and Leia and Lisa.
So there she was, ping-ponging back and forth between her husband and Leia and Lisa, washing her hands constantly and hoping desperately that she and “the girls” wouldn’t get sick. Bumbray-Graves didn’t know who would care for Leia and Lisa if she did. No one could fill in.
“That’s what I was thinking about the whole time. You know, if I get sick, who’s going to help me?” Bumbray-Graves recalls.
Worse, Bumbray-Graves couldn’t afford to get sick — literally. As a direct home care worker in Virginia, she is paid just over $12 per hour, with no paid sick leave or vacation time and no health insurance (she’s covered by her husband’s insurance). Her husband’s illness meant losing out on some of his wages, and their savings account had been decimated by badly needed repairs on their home’s roof and a furnace that stopped working for weeks in December.
Home care workers, certified nursing assistants and hospital aides are a precious resource in the local and national fight against the coronavirus. A year in, they’re exhausted, and still facing the grinding stress and fear of providing constant care, the strain of staffing shortages, and the trauma of losing patients and loved ones to COVID-19.
Like Bumbray-Graves, many of them are doing that work for modest to low wages. Some work multiple jobs to make ends meet.
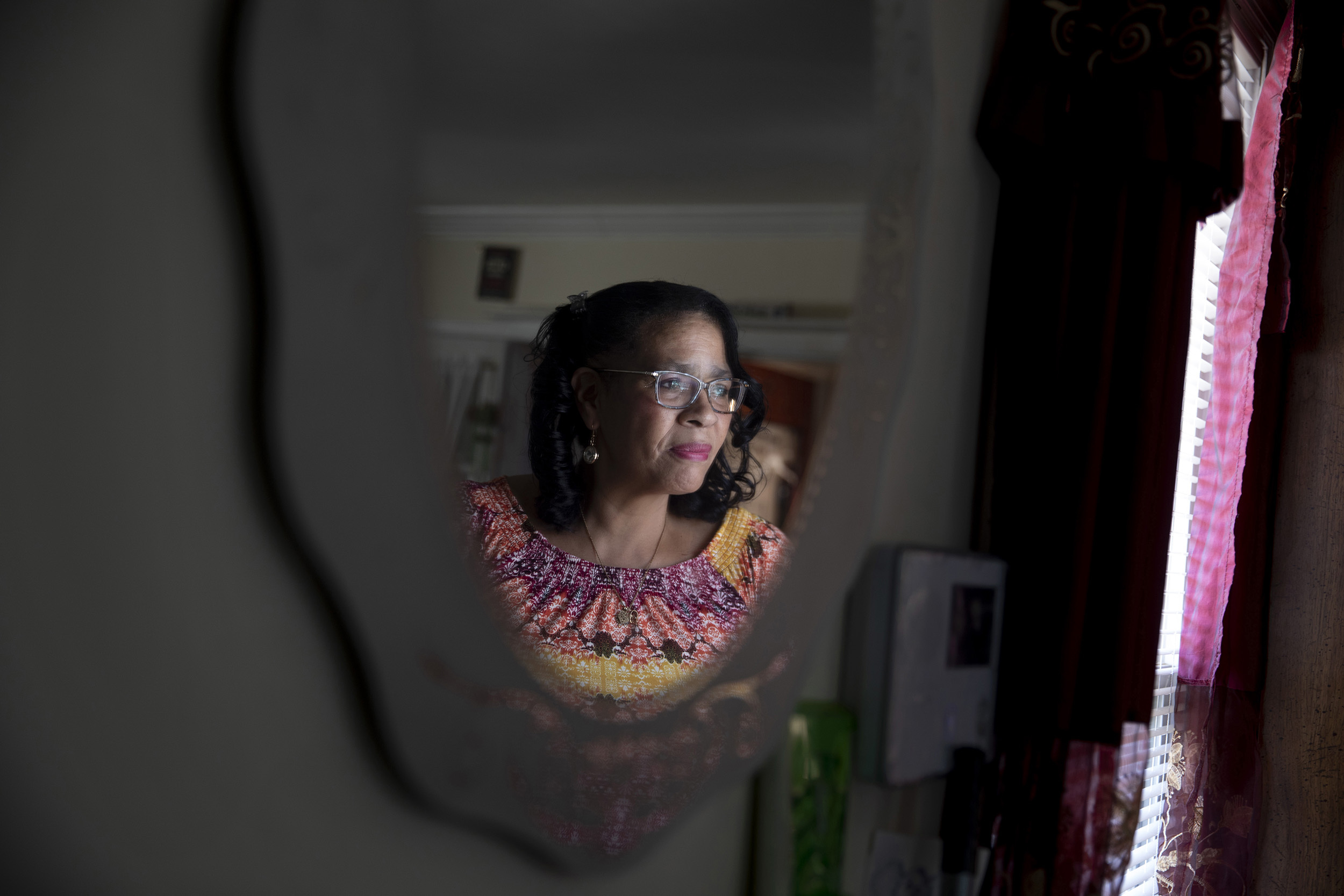
‘They’re not earning a lot’
Home care workers in Virginia currently make about $23,000 a year, according to federal statistics from 2019. Other health workers are facing the pandemic for similar wages. Aides in the Maryland long-term care facilities, which have borne the brunt of the pandemic make just under $30,000 a year.
Those wages often mean these frontline workers have to take long hours or multiple jobs to get by. Cyntira Gilchrist works close to sixty hours a week at one Maryland nursing home. She picks up shifts at another facility and spends the rest of her hours with a home care client. Gilchrist says she’s not sure how the math even adds up.
“Sometimes I can’t figure it out,” she told WAMU/DCist, speaking while she was with her home care client. “It just happens.”
Gilchrist takes pride in working hard to help others, a commitment she feels strongly about after a yearlong stint of being a patient herself. But she also worries about her own health sometimes, working so hard. She has a respiratory condition, and the long hours behind masks and other protective gear are hard.
“I love doing what I do, but doing what I’m doing right now, with this going on, it’s just that much harder on myself,” she says.
Long-term care facility aides taking on long hours or multiple jobs is far from unusual, a symptom of low wages and chronic staffing shortages in the industry. That’s according to Nancy Lerner, a University of Maryland professor and a former director of nursing at a Maryland nursing home.
“They’re trying to take care of their families, which means working, which often means working a regular job and then an extra job,” Lerner says. “They’ll work somewhere in the morning, they’ll work somewhere at night or in the evening.
“The only thing you could say that’s positive is that they still have jobs, but they’re not earning a lot,” Lerner says.
There are some modest improvements: many long-term care facilities have offered workers varying degrees of hazard pay during the pandemic. Other workers report receiving bonuses on top of overtime if they work longer hours.
In Virginia, the state is raising direct consumer home care workers’ pay by 7% over two years (it went up 2% last summer, and will increase by 5% in July), and the workers received a one-time $1,500 hazard pay payment in January. Legislation recently passed by the General Assembly would grant workers like Bumbray-Graves five days of paid sick leave, and this year’s state budget would raise wages again, by nearly 19%. Both now await a signature from Gov. Ralph Northam.
But David Broder, the president of SEIU 512, the Virginia union representing Bumbray-Graves and other direct consumer home health workers, says much more could be done to support them.
“What they need to stay safe then is what any frontline worker needs,” Broder says. “They need PPE. They need a living wage so that they’re not forced to work two to three jobs and go from home to home and take public transit and put themselves and their clients at risk. They need health care and they may need paid sick leave so that they can take care of themselves and their families as they take care of others.”
SEIU 512 successfully pushed for funding to give direct home care workers personal protective equipment like masks and gloves. But Broder says the program ended in January.
Bumbray-Graves agrees with Broder. She says her teenage granddaughter’s first job at $15 per hour paid more than the work Bumbray-Graves has dedicated her life to doing.
“We need benefits,” she says. “We need benefits because it’s a rare person that doesn’t ever get sick.”
‘It hurts you’
Hours and pay aren’t the only hardships facing aides and other health workers during the pandemic. Many describe the fearful emotional toll of facing down the virus every day at work.
Rhonda White is a certified medicine aide in a nursing home in Maryland, a job she’s been doing for more than two decades. At the beginning of the pandemic, she worked on a COVID-19 floor at her long-term care facility, taking care of very sick patients.
“It was a lot of anxiety, depression,” she says. “Not knowing what the COVID was [at the beginning] was the problem.”
Many workers in long-term care facilities develop real relationships with the residents. White and many others describe the pain of watching patients succumb to COVID-19.
“It hurts you because these are innocent people. They didn’t ask for what’s happening. They don’t know what’s going on, half of them,” she says.
Loss has been everywhere this year for people in these jobs. Gilchrist says one of her lowest moments of the pandemic was losing a resident who regarded her as a daughter.
“That just put a hole in me,” Gilchrist says. She’s been leaning on her faith as a Muslim for the strength to carry her through her grief and anxiety.
Lerner says aides in nursing homes and assisted living facilities typically get into the field and stay in it because they’re “natural caregivers” who develop deep relationships with their patients — even though their patients are often close to the end of their lives. The pandemic has accelerated that dynamic, with residents in nursing homes and assisted living facilities accounting for a big share of deaths from the virus.
“Often because of the no-visit policies, [the aides] are the ones who have to be with them when they die, much like a surrogate family,” Lerner says. “So they have that grief.”
Other workers have gotten sick themselves, after long hours exposed to the coronavirus — at the beginning of the pandemic, sometimes in used protective gear. Gilchrist’s cousin, another long-term care worker, contracted COVID-19 and died, leaving behind three children.
Tony, an emergency room tech who works the night shift at a hospital in Maryland, compares his experience in the ER this year to his military service in the Gulf War. (WAMU/DCist is not revealing his full name because of concerns about retaliation.)
“It’s the same, it’s just a different front,” he says. “You’re battling a disease process that’s wreaking havoc.”
Tony spends his night shifts with COVID patients, helping doctors intubate them, starting their IVs and even performing chest compressions for CPR. The pandemic battle, Tony says, comes with a lot of hard casualties. He hates seeing people die separated from their loved ones. But he also has to steel himself against feeling too much.
“I don’t want to sound cold. You just have to put yourself and your mindset in a different place, that you know what, you can do whatever you can do and you can do the best you can…to help the people that you can help and to be a professional as you can and give them to give them as much dignity as [you] can,” he says.
“That’s how I do it. And everything else, that, I just try to block out,” he says.
That toll redounds outward, to workers’ family lives, too. After his night shift, Tony rushes to his mother’s house, where he picks up his three children. He spends his days trying to parent them — but at a distance.
“I’m here, we talk,” he says. “But where you would go up and give your son a hug — I’m just mindful because I don’t want to bring anything [home to] my kids.”
Lerner says many long-term care aides face similar challenges, juggling parenthood and their work on the front lines.
“They are often, especially in urban areas, single parents. And as a result, they’re running two lives,” she says. “They also have to get their kids off to school in the morning or into some sort of childcare, so they have a lot of stressors.”
‘The struggle is for real’
Many lower-wage health care workers are people of color, from communities that have been hit disproportionately hard by the virus. All of the workers interviewed for this story are Black, and many have seen friends and family members sicken and even die in the pandemic.
While her husband was sick, Bumbray-Graves says she had 10 close family or friends who also had COVID-19. She’s lost several family members to the disease.
Broder, from SEIU 512, traces the burdens home care workers like Bumbray-Graves bear directly to structural racism and sexism. The field, he says, is 90% women, majority Black and Brown, with a significant immigrant population, too.
“The challenges we face in home care are the challenges we face when we devalue the work done by Black women,” he says. “ When important work is done by a workforce that’s predominantly women and often women of color, we don’t treat it with the same dignity and respect and we don’t fund it the same way. And that is a problem that’s really catching up to us.”
People of color make up about 40% of the health care workforce overall, according to an analysis from the Kaiser Family Foundation.
But Black and Hispanic health care workers make up a “relatively larger” share of aides, personal care workers, direct contact support workers, and home health care workers, per the analysis. Black workers account for a larger share of workers in residential long-term care settings, per the study.
Furthermore, “Black health care workers and their families are particularly likely to report certain [pandemic] impacts, including knowing someone who has died from the virus and a negative impact on their ability to pay for basic needs,” according to the same report.
And there’s evidence that workers of color are more likely to get sick. A study published in July found that health care workers of color reported higher rates of reuse or bad access to personal protective equipment. A CDC analysis of the pandemic’s effects on medical workers in a multistate hospital system in April and June found higher rates of COVID-19 antibodies in workers of color than in their white colleagues.
This year’s movement for racial justice has been on Bumbray-Graves’s mind. She sees her struggles in the struggles of the civil rights movement and the protests against police brutality toward Black people that followed the police killings of George Floyd and Breonna Taylor.
“I’ve been watching some Black history programs lately that have made me cry because the struggle is for real,” she says. “It’s been going on forever, and then we have to have a new struggle of fighting with the union constantly just to get some benefits for us.”
Bumbray-Graves loves her job. She loves playing word games and doing puzzles with Leia. But she also feels her work is shortchanged and undervalued.
“What we do is essential. Someone has to do it,” she says. “The people like us, we do it from the heart, because it has to be done whether we get paid what we deserve or not.”
Low pay, long hours, the loss of her savings, her frightening brush with the coronavirus, the police shootings of Black people, the white supremacy on display in the Capitol insurrection: it’s all left her exhausted.
“We have had enough. We’ve had enough. We always have to fight for everything,” she says.
This story has been updated to include information about the proposed Virginia state budget.
 Margaret Barthel
Margaret Barthel



