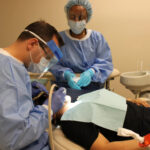
Mary’s Center laid off 48 employees, 6% of total staff in recent weeks — an unprecedented move in the prominent D.C. community health center’s 33-year history.
CEO Tollie B. Elliott Sr. says they decided to reduce staff to operate more “efficiently,” adding that the center foresaw financial challenges with pandemic-era relief ending and supply costs continuing to rise.
“Although we’ve never gone through this, this is not unique to Mary’s Center. It’s not unique to the D.C.-area. It’s something that’s happening across the country, in many different sectors,” Elliott tells DCist/WAMU.
While Elliot says there are no more planned staff reductions, multiple current and former employees say they’re concerned about what the layoffs mean for the future of Mary’s Center, clinics that provide a blend of health care and social services to tens of thousands of Washingtonians, many of whom are poor or people of color. Some of the employees, who all requested anonymity for fear of retribution, say the elimination of critical staff could make it harder for them to do their jobs as effectively while others worry that people might quit in the coming months because the layoffs were such a demoralizing experience.
There’s disagreement amongst leadership and some staff about whether layoffs will impact patients, many of whom are likely already impacted by the end of pandemic-era relief, from food programs to housing assistance.
While the health sector across the country has seen some job eliminations in recent weeks, local community health centers like Mary’s Center are particularly worried about trying times in the months to come as the country moves on from COVID-19 and support for their work reduces.
Mary’s Center played a critical role in the D.C. region’s response to the pandemic, vaccinating at least 27,000 hard-to-reach yet vulnerable people and helping to reduce economic and racial disparities in the vaccinations. The Obama Administration awarded its founder Maria Gomez the presidential citizens medal and the Biden Administration invited clinic staff to the White House to discuss their successful vaccination efforts.
Staff say the timing of the layoffs stings given the years they’ve spent as frontline workers – work they describe as exhausting and even traumatizing.
Mary’s Center employees learned of layoffs in a March 17 email, shared with DCist/WAMU, and said individuals were provided severance based on their tenure. After comparing notes between departments, a longtime staff member says they learned that several people within the behavioral health department, who were middle management but sometimes saw patients, as well as many nutritionists and health educators had been laid off. Mary’s Center treats the overall wellbeing of their patients, offering therapy and specialized services like nutrition education classes and cooking demostrations alongside more traditional health care provision, like routine check-ups and vaccinations.
“Mary’s Center is not Mary’s Center without strong social services,” says the staff member.
Another staff member who’s been at Mary’s Center for nearly a decade says some of the people let go played an “outsized role” at the organization. “It was, like, shocking to see those names. People who are really dedicated. The last people in the world who you think would be fired,” they said.
One laid off individual says they were blindsided. They requested anonymity, fearing their severance package could be jeopardized. The former staffer says their experience with the layoffs — no notice, a brief phone call with management, and a ban from returning to the office — contrasted with their time at Mary’s Center, where leadership often purported the workplace to be a family.
“Not being able to say goodbye to colleagues and patients who I worked with for a long time… To have my years of service at Mary’s Center come to an end in that way was hard,” they said. “Then figuring out what’s next. I’m suddenly looking for work for the first time in a long time.”

Mary’s Center has become a trusted resource since opening in 1988, Gomez started offering prenatal care to Central American immigrants fleeing war and poverty. The health center has greatly expanded since those early days in an Adams Morgan basement to several locations across D.C. and Montgomery County.
Elliott says they are “still 800 strong” and can fulfill the center’s mission because the layoffs were strategic. He says that layoffs were predominantly among administrative roles and therefore weren’t patient-facing. However, there were several individuals who provided social services to patients, like counseling, and they had significant years of experience. Elliott says the laid-off staff’s “low volume” of patient care has been absorbed by other staff with space in their schedules.
“The actions taken, although difficult, are an appropriate and mature response to the environment that lays ahead of us,” says Elliott, who became the CEO in 2022 after the founder retired.
Multiple former and current Mary’s Center staff say they are still concerned about the priorities under new leadership and wonder why Mary’s Center didn’t better prepare for the end of pandemic-era funding and continued to hire or promote people, including several senior administrative positions, as recently as last year. They also want to know if Mary’s Center seriously considered other cuts before layoffs, including a salary reduction of the highest-paid staff.
Elliott, who previously served as the chief medical officer, says he sought to address financial challenges through other cuts before layoffs, such as switching to a less expensive vendor for the call center. Elliott also says that grant constraints mean certain funding can only be spent on specific staff and services. He expects to hire more people for a new location in Prince George’s County, for example, money earmarked due to the high need there.
Like other federally-qualified community health centers, Mary’s Center saw a significant boost in government grants over the last couple years, particularly due to the federal CARES Act and American Rescue Plan. Mary’s Center overall staff grew by roughly 10% during the pandemic.
The nonprofit ended 2020with $5.7 million in revenue leftover — the first time it hadn’t run a deficit in several years,according to audited financial statements. In 2021, Mary’s Center ended with $4.7 million in revenue, after accounting for expenses. But the last round of American Rescue Plan dollars expired last Friday, unless centers requested an extension, which Mary’s Center spokesperson Lyda Vanegas says they’ve done in order to spend down the “small amount” left over.
CEOs of other local community health centers say the end of ARP dollars make their work harder to sustain but so do other sunsets in pandemic relief. For example, people with Medicaid insurance will no longer be continuously enrolled beginning this month because federal enhanced dollars to state governments end. Individuals could become uninsured because they forget to re-enroll or have become ineligible when they try to. An estimated 30,500 D.C. residents are expected to lose coverage.
“There’s a confluence of factors,” says Catalina Sol, the executive director of La Clínica del Pueblo. “The continuing challenges to our workforce, to our health sector, the huge need, more need than ever, [among] our patients — those put immense pressures on health centers.”
Local community health centers will treat uninsured patients – one in five community health centers patients nationwide are uninsured – even though insurance is a major source of funding. Sol says at least 33% of their patients are uninsured. Elliott says Mary’s Center saw $7.2 million in uncompensated care last year.
Local community clinics La Clínica del Pueblo, Community of Hope, Whitman-Walker Health, and Unity Health Care all say they do not foresee a reduction in staff or services due to a myriad of reasons like private funds or staff vacancies.
Community of Hope CEO Kelly Sweeney McShane says they are still spending down ARP dollars after receiving an extension. They’ve also had unspent revenue due to vacancies. Still, they foresee difficulties given a confluence of factors, including their patients or staff losing enhanced food and housing assistance. The CEOs also worry about their own workforce, who are reeling from burnout and trauma associated with the pandemic.
“While COVID feels like it’s over, there are still a lot of challenges and a lot of ripple effects from COVID,” says McShane.
 Amanda Michelle Gomez
Amanda Michelle Gomez