In Northern Virginia, the likelihood that you’ll live to the age of 75 mostly hinges on your racial and ethnic background and what neighborhood you live in, according to a new report from researchers at Virginia Commonwealth University.
Race, ethnicity, and neighborhood were also major factors in determining whether you died from COVID-19 between 2020 and 2021, the report found.
“For people of color, the pandemic made a bad situation terrible,” said Steven Woolf, the lead study author and director emeritus of VCU’s Center on Society and Health, in a press release. That was particularly true if the person of color lived in a higher-poverty, historically-disadvantaged neighborhood.
In the report, Woolf and his co-authors call on local officials to act, funneling resources and putting in place policies to address the history of racial discrimination that has created wide disparities among residents, in life and in death.
The study, funded by the Northern Virginia Health Foundation, looked at death rates and the likelihood of premature death — before 75 — across Northern Virginia jurisdictions, by county, General Assembly district, and census tract. It compared data from 2015-2019, before the pandemic, to data from 2020 and 2021, in the initial two years of the global health crisis.
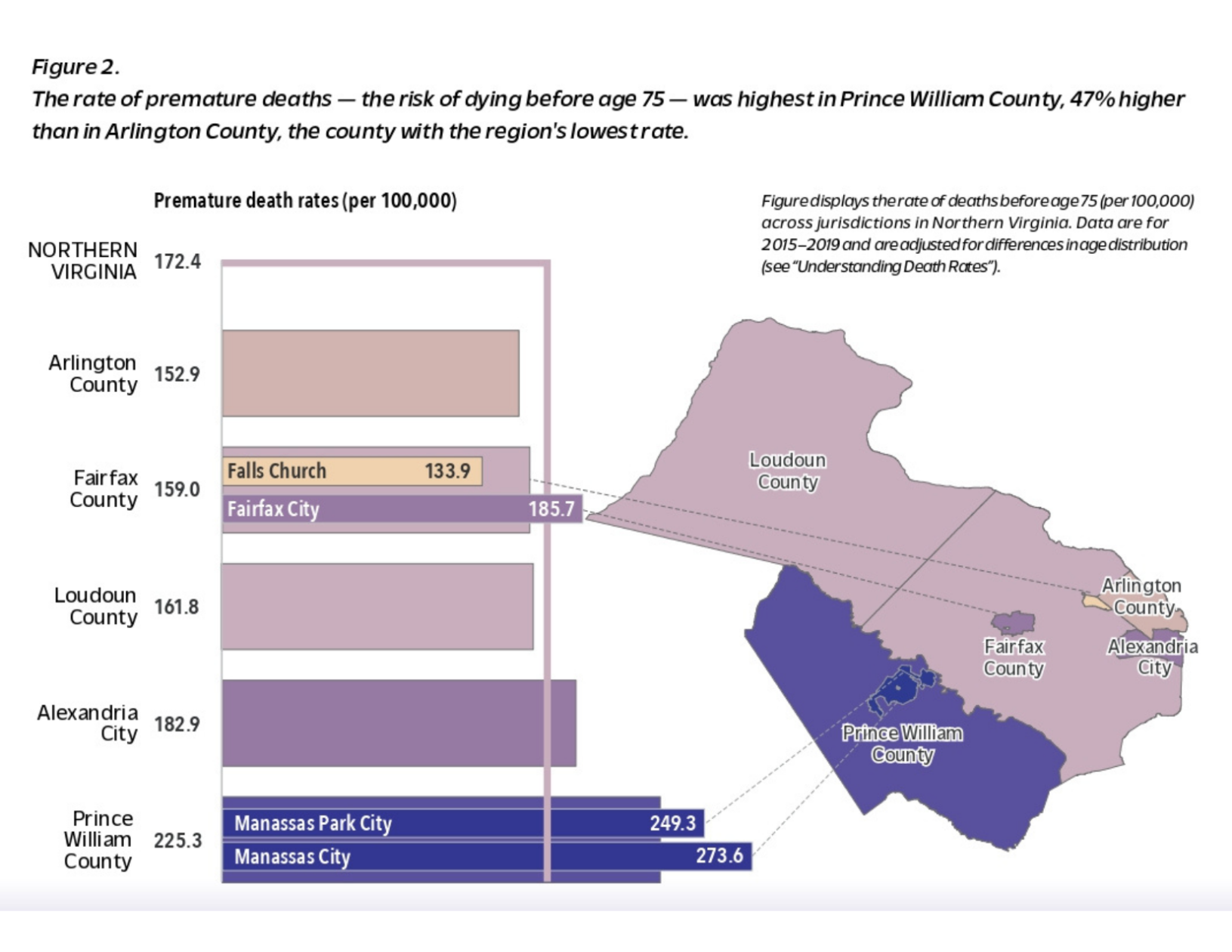
From 2015-2019, residents of Prince William County were most likely to die before the age of 75 compared to residents in other jurisdictions, though specific neighborhoods with high death rates are distributed across Northern Virginia. Census tracts in Manassas and southern Prince William County; Leesburg and Sterling in Loudoun County; Annandale/Springfield, Herndon/Centreville, Seven Corners/Bailey’s Crossroads, and Route 1 areas of Fairfax County; the Shirley Highway (I-395) corridor; southern Arlington County; and downtown Alexandria all had the highest premature death rates.
Black people were 44% more likely to die before 75 than their white counterparts — and that gulf gets wider or narrower depending on where you are in the region. In Arlington and Alexandria, that percentage shoots to nearly 120%; in Prince William County, it’s 9%, and in Loudoun County, it’s 28%.
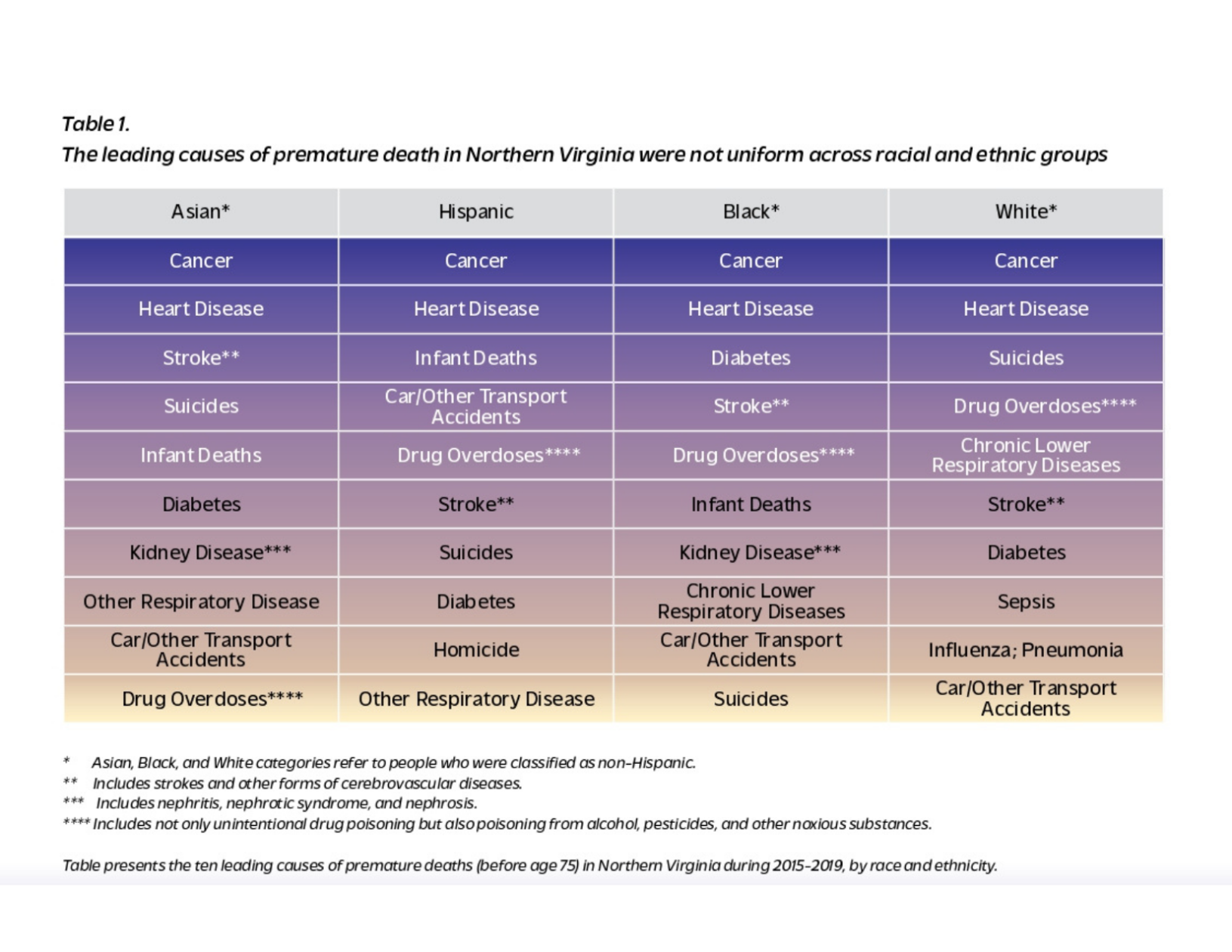
Two-thirds of Northern Virginia’s premature deaths before the pandemic were preventable, per the report, because they were linked to a lack of preventative services or good medical treatment. The leading causes of death were cancer and heart disease across the whole region, but other main causes of death varied widely depending on where someone lived and the person’s race and ethnicity. For neighborhoods with lower death rates, suicide tended to rank third, higher on the list; neighborhoods with higher death rates generally ranked strokes, diabetes, and drug overdoses higher
Causes of death also varied by race and ethnicity. The fourth leading cause of death for Hispanics in Northern Virginia between 2015-2019 were injuries from being struck by cars or other vehicles, which ranked considerably lower for white people, Black, people, and Asian people.
The vast differences in when and how people die early are mostly due to the social and environmental factors affecting people’s lives — “sharply divergent socioeconomic conditions,” as the report puts it.
“High death rates often exist in places with limited access to education, income, wealth, and employment and where residents face adverse environmental conditions that affect health, such as inadequate access to affordable housing, food, health care, and transportation,” the report notes.
The research builds on previous work on Northern Virginia’s “islands of disadvantage.” These are neighborhoods where high poverty rates and poor access to things like education, economic opportunities, transportation, and health care contrast sharply with the region’s overall good outcomes.
A 2021 study traced how a history of racist policies like segregation, restrictive covenants in housing, and underfunding of schools serving Black children continues to affect the prospects and health of residents of color today. It also noted that some of the wealthiest and healthiest parts of Northern Virginia are areas that benefited from historical racial discrimination, allowing residents in those areas to concentrate multigenerational wealth and power in their neighborhoods.
Often, these “islands of disadvantage” with high premature death rates sit right next to neighborhoods with some of the lowest rates. The Bluemont and Buckingham neighborhoods in Arlington, off Arlington Boulevard, are separated by a single road: North Henderson Road. But despite their close proximity, the premature death rate in Buckingham is five and a half times that of Bluemont.
That’s a less surprising finding when you consider the context on either side of the road, the report argues. The median household income in Bluemont was five times higher than the median in Buckingham, and the poverty rate in Buckingham is seven times higher than in Bluemont. In Buckingham, the rate of uninsured people was 70 times greater than Bluemont. Bluemont residents are 50% more likely to have a bachelor’s degree. Buckingham’s population is about half Hispanic, Black or Asian people, while people of color accounted for less than a third of Bluemont residents.
“These patterns are not unique to Bluemont and Buckingham,” the report is quick to point out. “They recur throughout Northern Virginia.”
The pandemic made it all worse. COVID-19 became the third leading cause of premature death in Northern Virginia in 2020 and 2021, and that toll fell unequally.
COVID death rates for Black people were more than double those of white people in Northern Virginia, and nearly double for Hispanics, for whom the pandemic became the leading cause of people dying before age 75.
COVID increased death rates in the area overall — except in the wealthiest parts of Northern Virginia, which saw no increase in death rates.
Prince William County had the highest COVID death rate, and most neighborhoods with high premature death rates before the pandemic also had high death rates due to the disease.
Those “islands of disadvantage” became “hot spots” for the spread of the disease, as the report puts it. They also bore the brunt of economic effects like job loss and housing insecurity. In fact, COVID death rates for people of the same race or ethnicity could be twice as high in some neighborhoods as in others.
The pandemic also shifted how people died prematurely overall in Northern Virginia, with a nearly 50% increase in deaths due to alcoholic liver disease and a 40% increase in drug overdoses. There were decreases in premature deaths due to infant mortality, falls, sepsis, Alzheimer’s disease, and the flu.
The report calls for public policy and investments — in affordable housing, economic development, better health care access, public health departments, and public transportation, for example — targeted at improving social and economic conditions in the region’s “islands of disadvantage.” It also advocates for acknowledging the effects of systemic racism, in history and in current public policy.
 Margaret Barthel
Margaret Barthel