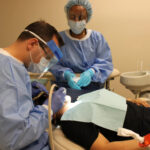
Mary’s Center, a clinic in D.C. that serves more than 60,000 patients a year, has been at the forefront of the region’s response to the coronavirus pandemic.
In partnership with the D.C. government, it has tested over a thousand people for the virus. When Mary’s Center opened a free testing site in Brightwood earlier this month, they were able to test 300 people within the four hours they were open.
“We could have seen people all day long,” says Mary’s Center President and CEO Maria Gomez.
And the work goes beyond medicine. The clinic has helped distribute cash assistance to immigrants who are ineligible for federal stimulus payments.
But Mary’s Center, and clinics like it, may need their own stimulus payments soon.
Mary’s Center is what’s called a federally qualified health center, meaning it provides primary care to patients regardless of their ability to pay. About 200,000 D.C. residents visit such health centers each year. But while demand for COVID-19 tests is high, regular visits to these clinics have plummeted, leading to a steep drop in revenue.
The problem is most acute for the clinics with large numbers of Medicaid patients, where balance sheets depend on people coming in for regular visits and the public insurance program reimbursing providers for those visits. Without support in the form of federal relief or a revised funding model, these clinics — and a crucial part of the city’s health care infrastructure — are in danger.
“Financially, we’re hurting deeply,” Gomez says.
Medical and behavioral visits to health centers across the city were down anywhere from 40% to 75% last month, and about 30% this month. The D.C. Primary Care Association, an advocacy group whose members include 15 community health centers in the District, told the D.C. Council last month the clinics were collectively losing $1.1 million a week.
D.C.’s Medicaid program has begun reimbursing telemedicine at the same rate as in-office services, but this is a temporary measure, for now, and not enough to make up for the shortfall.
This drop in revenue comes at a time when clinics are proving themselves particularly essential to public health. Several target their free walk-up testing towards Latinx and black residents, who face some of the highest rates of infection and death from the virus. Beyond COVID-19, the clinics have been proactively reaching out to patients to make sure they do not fall behind on management of chronic conditions.
Some health centers in the D.C. region have applied for federal loans, but some of the larger clinics have too many employees to be eligible.
Mary’s Center, for instance, employs about 730 people and is ineligible for the federal Paycheck Protection Program, which is limited to businesses with 500 or fewer employees. Mary’s Center has received financial support from foundations and individual donors, but Gomez says she is drawing from the organization’s reserves.
“That leaves us pretty empty at the end of June,” Gomez says.
Gomez has been hesitant to seek other forms of federal relief during the crisis. For example, the government is now reimbursing providers for coronavirus testing and for care for the uninsured — as many as 35% of Mary’s Center patients are uninsured — but this requires clinics to ask for each patient’s social security number or driver’s license information.
“We have to give really private information to the government,” Gomez says. “And so we are debating as to whether we can use that money to subsidize our uninsured patients, because so many of them are not documented.”
Unity Health Care, which employs about 1,000 people and treats 100,000 patients a year, is another large health center that was unable to apply for the Paycheck Protection Program. Health care workers with Unity work at several clinics throughout the city and also in the D.C. Jail and homeless shelters. CEO Vincent Keane estimates Unity’s clinics have seen 5,000 fewer patient visits a month for the last two months, despite eased restrictions on telemedicine.
Keane says Unity’s monthly losses are between $500,000 and $700,000.
“Unfortunately, in today’s health care world, that’s how we still generate revenue — by visits,” Keane says.
Unity has received some assistance through the federal CARES Act, which has helped to fund COVID-19 testing efforts and personal protective equipment for staff, but it’s difficult to know if or when other forms of federal assistance might arrive.
Keane says the federal assistance is “filling gaps,” but he sees it as a one-time infusion of funds, not a permanent solution.
This precariousness is a setback for a city that has worked to expand its health safety net in recent years, opening new state-of-the-art facilities in neighborhoods with some of the worst health outcomes.
“We’ve spent the last 20 years building primary care infrastructure in this city,” D.C. Primary Care Association chief executive Tamara Smith said last month. “Everything we spent the last 20 years building is in jeopardy, because the revenue is not coming in.”
Smith says clinics have received about $12 million dollars in federal money, which they used to expand testing capacity, reconfigure their facilities and ramp up telemedicine. She says she’s turning her focus to the “long haul” now, and determining how clinics can keep their doors open in the coming years.
One potential solution would be a system of retainer payments — money from the federal government that is not tied to the amount of patient care clinics are delivering. Medicaid directors from across the country requested such payments in a letter to the Center for Medicare and Medicaid Services and the Office of Management and Budget last month.
Sara Rosenbaum, a professor of health law and policy at George Washington University’s school of public health, says these retainer payments would be the “fastest way to infuse money into the health care system that serves the most vulnerable people.”
And there’s local evidence that retainer payments could help, at least during a crisis. Federally qualified health centers in Montgomery County are facing a similar decline in patients as D.C.’s clinics, but are buoyed by a payment system that’s similar to what Medicaid directors have requested.
These clinics treat patients who are part of a program called Montgomery Cares. It offers primary health care coverage for residents who are ineligible for Medicaid, Medicare and other forms of health insurance. Program administrators decided at the onset of the pandemic to reimburse primary care clinics for their services at pre-pandemic levels.
Dr. Cesar Palacios, executive director of Proyecto Salud in Montgomery County, says these payments are “a good help.” About 90% of the patients served by the organization’s two clinics are covered under the Montgomery Cares Program.
D.C.’s Department of Health Care Finance, which manages Medicaid in the District, is planning to ask for federal approval for a plan to give the city’s clinics a similar set of monthly payments through the end of the public health emergency. Under this plan, the Department of Health Care Finance would finance 30% of a monthly payment system, and the federal government would have to decide to pick up 70% of the cost for the payments to bring health centers back closer to pre-pandemic Medicaid revenues.
“Our goal is to ensure that we are able to support our District providers to ensure a sustainable healthcare system during and after the [emergency],” a Department of Health Care Finance representative says.
Meanwhile, as the clinics navigate financial uncertainty, they remain the primary safety net for residents with the highest risk of contracting the coronavirus.
“We’re able to provide really culturally competent care for people who are scared and often who are the ones who are in very crowded working conditions, very crowded living conditions and they’re critical infrastructure workers,” says Dr. Jessica Boyd, chief medical officer with Unity Health Care.
Moving forward, Gomez says she sees Mary’s Center as essential to expanded testing and contact tracing efforts. But a significant share of the work is also about providing patients who are facing enormous financial, emotional and health burdens with the support they need to make it through this crisis.
“Many of our providers have heard from some of their patients saying, ‘You know, it’s just too much. I can’t bear it. It’s not really worth living anymore,’ ” Gomez says. “So we’ve got to be that beacon of hope, and we’ve got to see that light at the end of the tunnel.”
 Jenny Gathright
Jenny Gathright