Lauren Fox has been a Capitol Hill resident for three years, and while she’s had allergies for all of them, she swears this year is worse than ever before.
“I’m just hacking up like a terrible cough. My nose is running. I even have a saline spray in the kitchen,” Fox said, gesturing to her inhaler, eyedrops, and the other medicines she’s relied on to get her through spring
Fox spoke from her Capitol Hill apartment on one of the lowest pollen count days of April, thanks to a rainstorm that washed away her pollen prison. But the relief was only temporary. Fox still felt the lingering effects of the congestion and cough she’s had all season. She was even diagnosed with asthma for the first time this year.

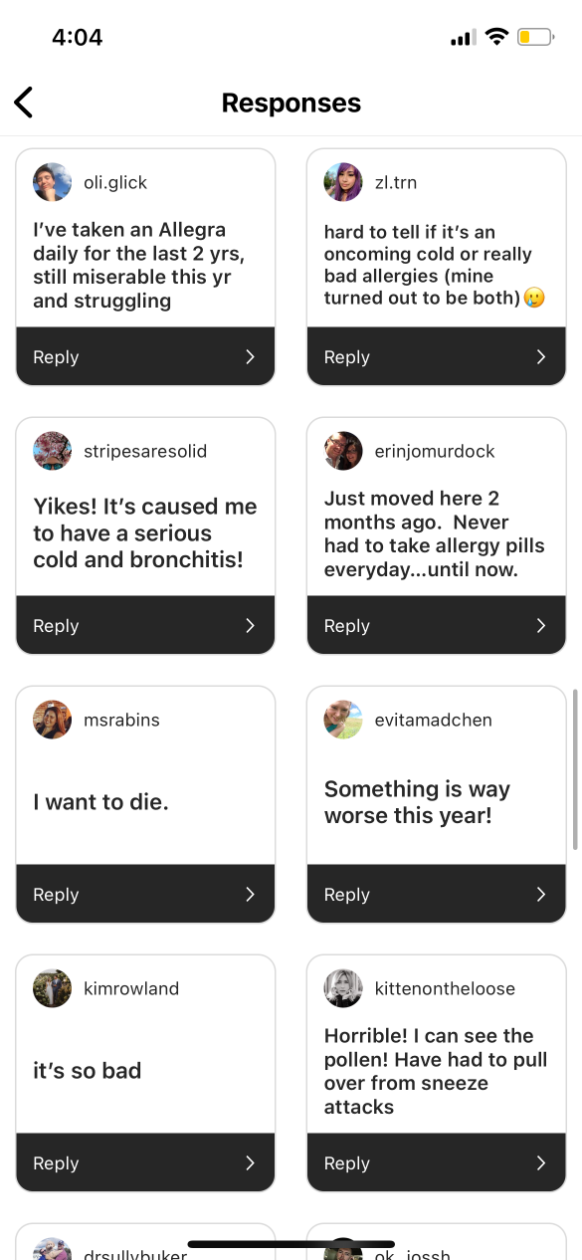
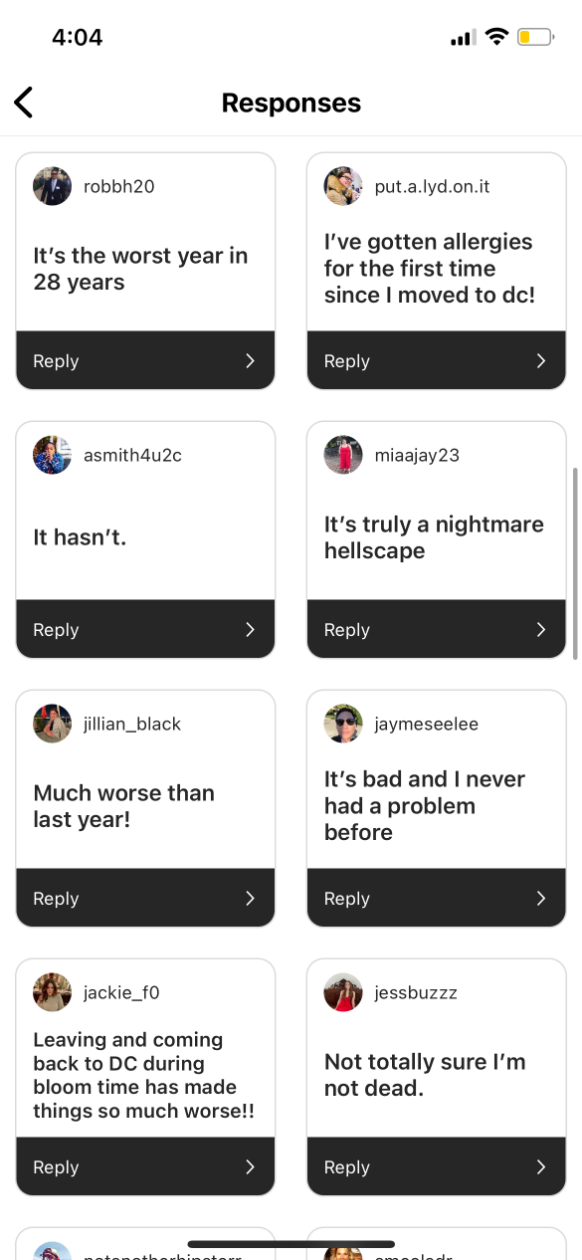
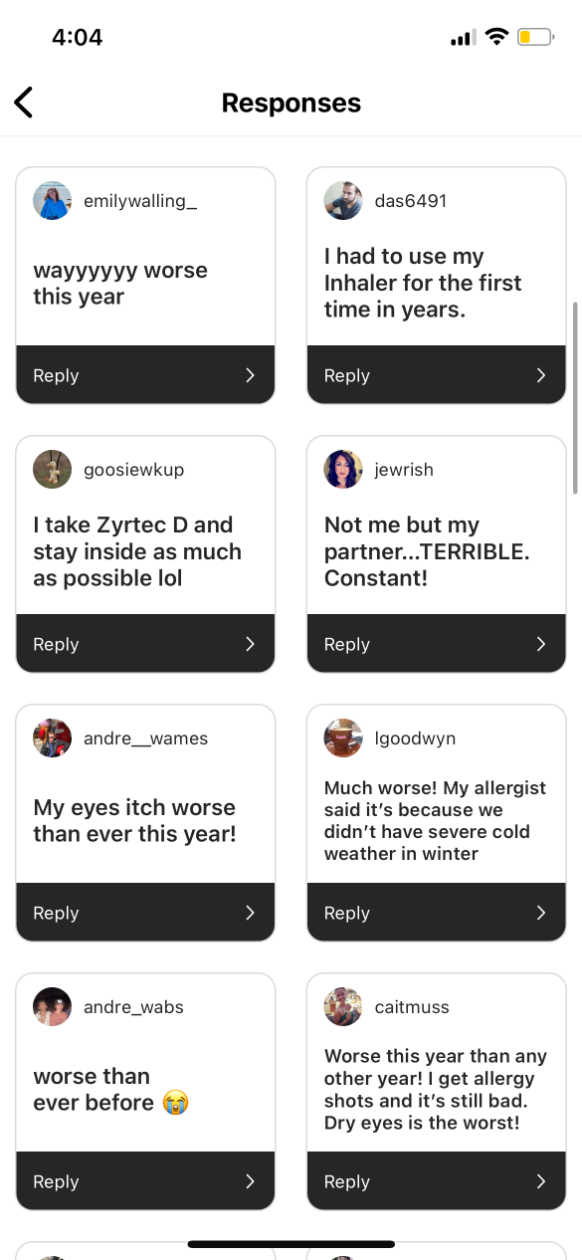
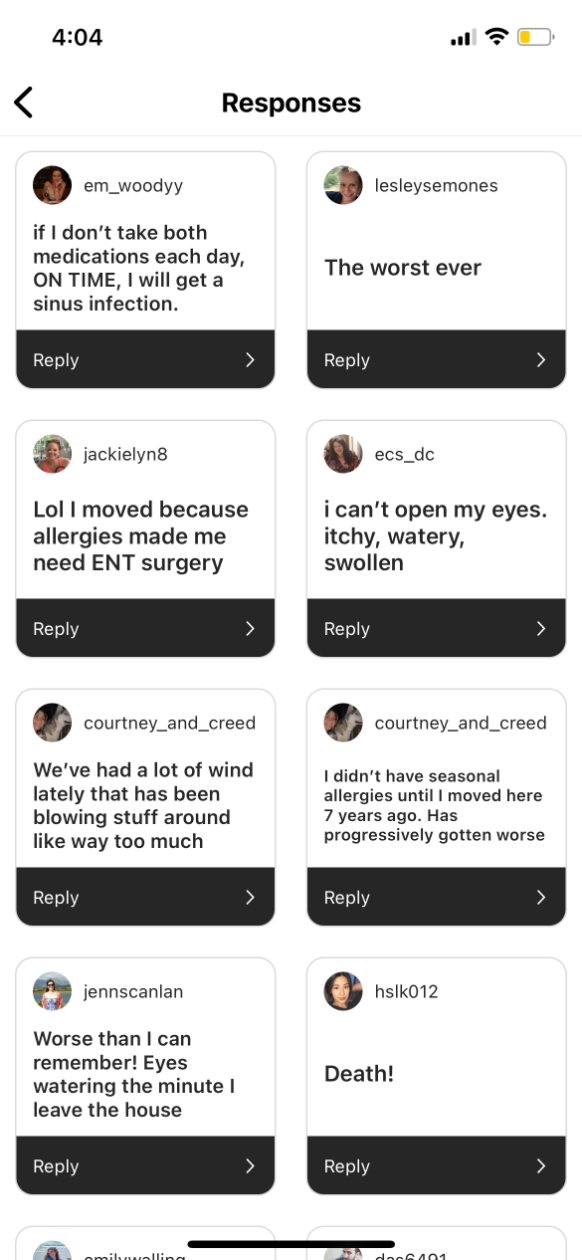
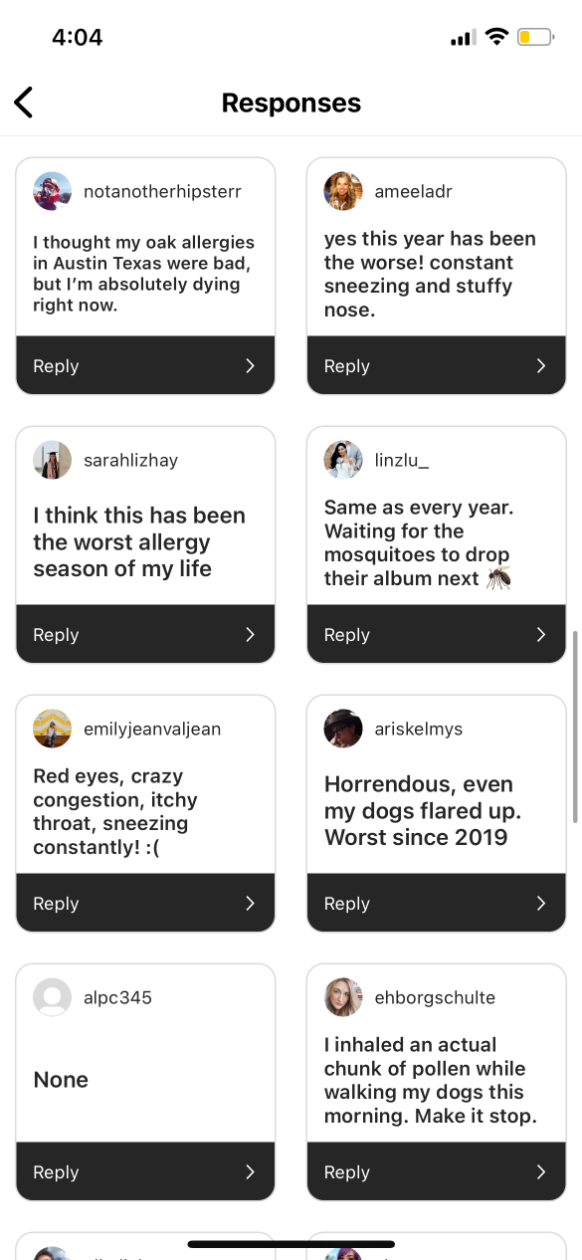
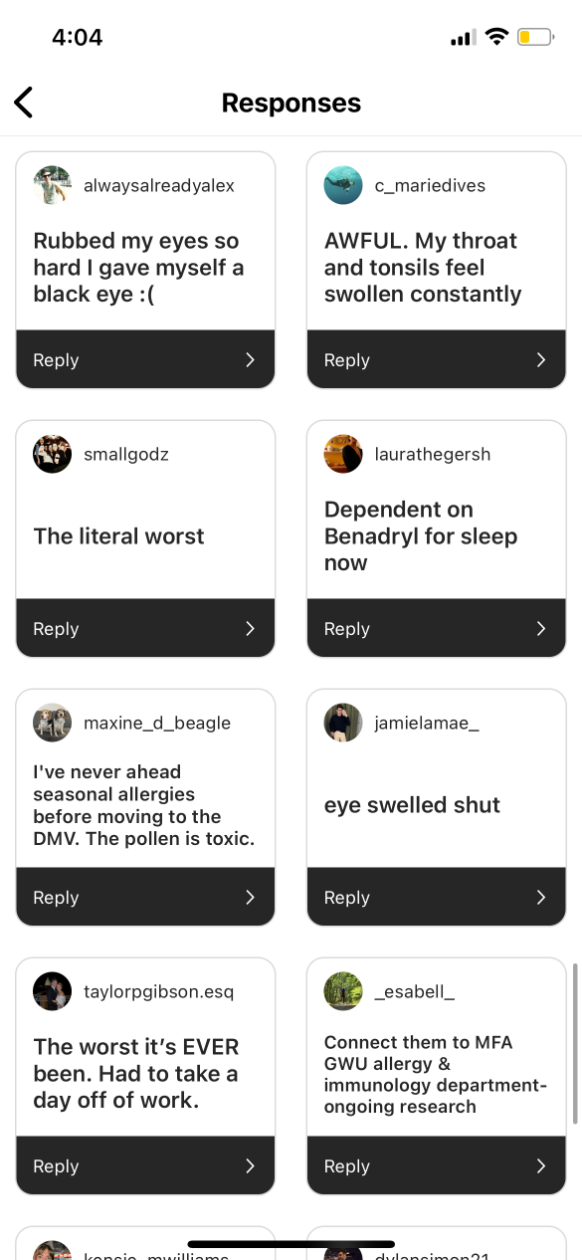
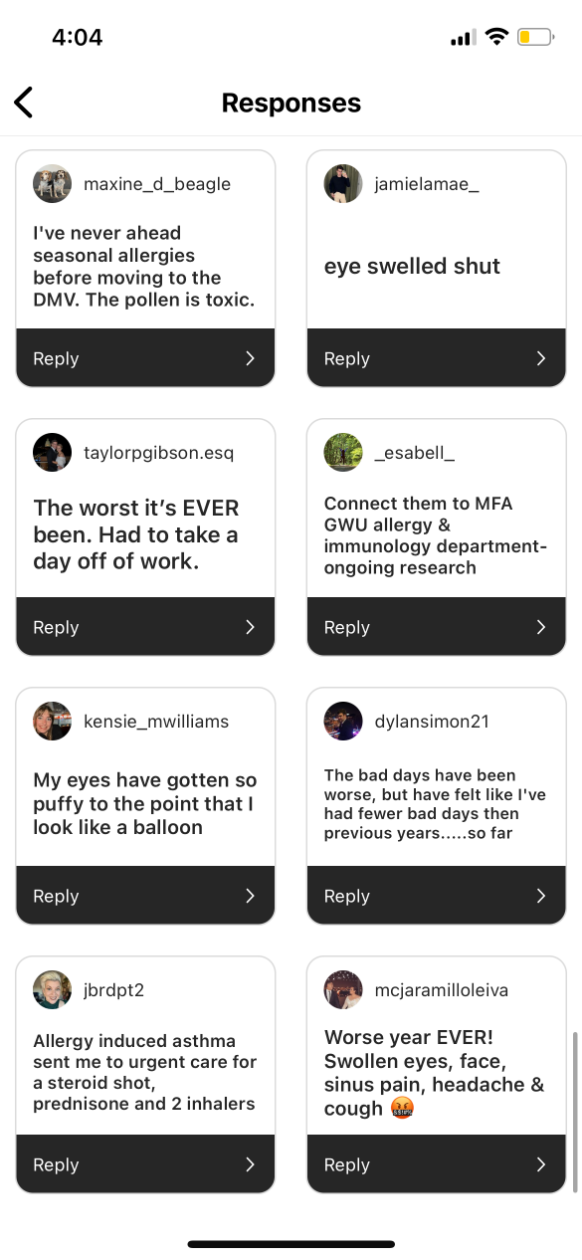
Fox isn’t imagining things — and she’s far from the only one suffering. Eyes swelling shut, swollen tonsils, being unable to leave the house, feeling “not totally sure I’m not dead,” D.C-area residents are having a difficult spring. Even some of the city’s dogs are experiencing symptoms. Thanks to climate change, things are, in fact, getting worse, and, like many healthcare problems, these issues aren’t felt equally across the city. Those without access to good healthcare, particularly primary care, can have a harder time managing allergy season.
But there is good news: both doctors and the allergy-prone say there are solutions to help make it to the summer months (just in time for mosquito season).
Here’s how residents responded to our survey:
“The two main sort of correlations between climate change and pollen allergies is that the pollen allergy season is longer than it used to be,” says Dr. Neelu Tummala, Assistant Professor of Surgery at George Washington University School of Medicine and Health Sciences and co-director of the Climate Health Institute at George Washington University. “On average, in North America, the pollen allergy season is about three weeks longer now than it was 30 years ago. And then there’s more pollen in the air.”
Tummala says that compared to three decades ago, there’s about 21% more pollen in the air, according to Proceedings of the National Academy of Sciences (PNAS). This is in part because the ground thaws earlier in the year now, so trees are able to grow earlier. Trees also use the greenhouse gas carbon dioxide, so when there’s more of it in the atmosphere, trees and plants grow more and produce more pollen.
And residents are feeling the pain. Emily Soule, who has lived in Dupont Circle for three years, says that this is the worst spring she’s ever experienced.
“I feel like every year I forget how bad my allergies are because I have like an off-season in the winter, and I’m like, ‘Oh, maybe this is the year that I’m no longer allergic to the world.’ And then I am rudely reminded every March that is not the case,” Soule says. “It’s funny because when everybody flocks to D.C. for the cherry blossoms, that’s my cue to tap out.”
Even her dog has been impacted by the pollen counts. And the sniffly nose and congestion aren’t just annoying, they can change her lifestyle for the season, making it difficult to manage symptoms and work.
“There’s no consistency level to it. I can wake up one day feeling totally fine, and the next day I literally feel like I have the flu,” Soule says. “I’m lucky that I have a flexible job, but it’s not like I can just take a sick day whenever I have allergy symptoms.”
New to the D.C. region? You’re probably suffering
Both Fox and Soule moved to D.C. fairly recently, and it’s common for people moving from other places to feel worse allergies after moving to D.C.
Eslam Chalabi moved to D.C. from Egypt in 2018. He’s dealt with allergies his entire life and was always careful to avoid sandstorms in his childhood. But after moving to the U.S., he discovered allergies could be worse than anything he’d ever experienced in Egypt.

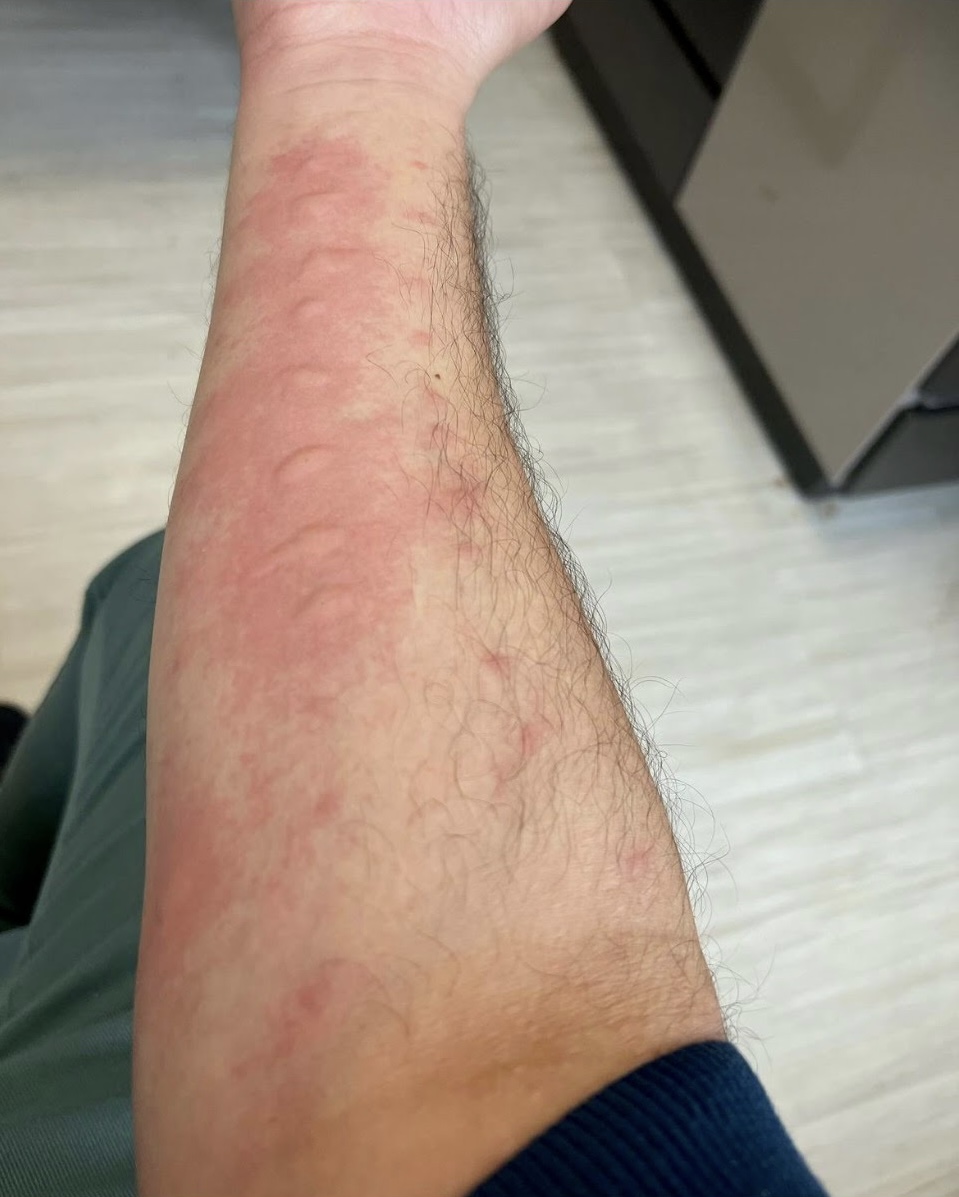
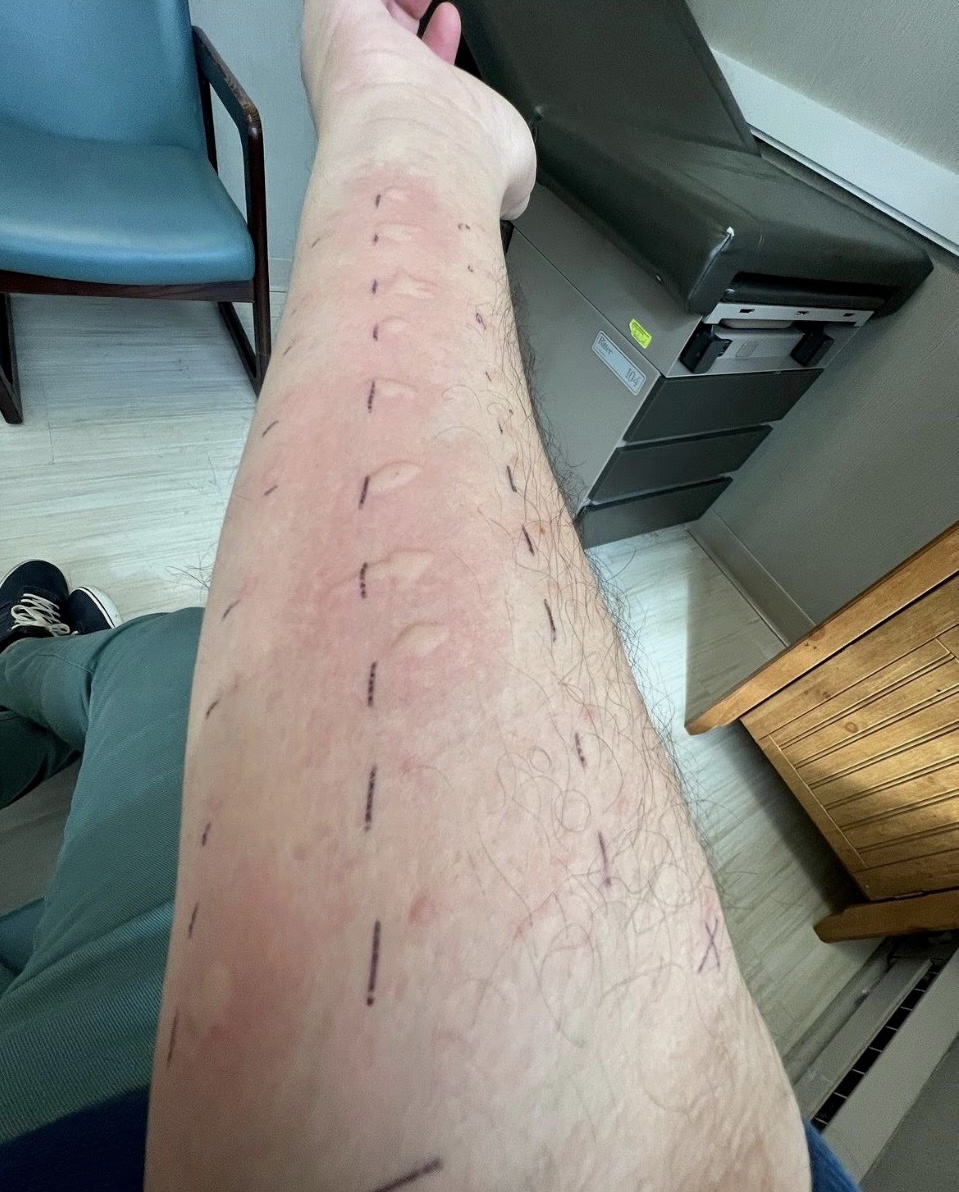
Chalabi described his first-ever allergy test in the States, typically administered by pricking small amounts of different allergens into the patient’s arm.
“My arm lit up like Cairo streets in Ramadan,” Chalabi says.
It felt like he tested positive for everything: house dust, mice, cats, dogs, horses, and, of course, this seasons’ bane: tree pollen. Chalabi has nasal spray, an inhaler, and eye drops, but his symptoms were so inhibiting he’s started getting allergy shots.
“Things have improved this year compared to last year. However, I had an anaphylaxis reaction [to the allergy shots], which was also not fun,” Chalabi says.
Despite the risk, Chalabi is still able to get the procedure done by bringing his Epipen and receiving lower doses. The procedure requires visiting the doctor once a week and then biweekly after a year. But he says the doctor’s visits are all worth it for relief but that he’s not immune to the struggles with insurance and getting medicine.
“It is very frustrating for me, especially because I’m still getting used to how everything works in the states, especially insurance and health insurance,” Chalabi says. “It’s like $200 for each medication. And I’m like, I have at least three that I’m going to use every month, if not more.”
Disparities in getting treatment
Drug costs can be a concern, especially for residents without insurance. And while D.C. Medicaid does cover most allergy medications, navigating the paperwork and finding the time can be difficult.

“It’s not that easy to just walk up and get the medicine; somebody has to approve that,” says Dr. Jessica Henderson Boyd, president and CEO of Unity Health Care.
But allergy care is also intertwined with primary care, something that not all D.C. residents have regular access to. And while they’re not the same phenomenon, allergies are related to asthma, a medical condition that affects children in poorer, more densely populated neighborhoods at higher rates. Nationally, Black and Hispanic children experience childhood asthma at higher rates across neighborhoods of any income. In D.C., poor housing conditions further exacerbate asthma.
“Allergies and allergens are a major trigger for asthma exacerbations, so once your body inhales those allergens, it’s going to react,” says Boyd.
For people experiencing either or both phenomena, primary care deserts in D.C. mean that many residents don’t experience consistent care.
Director of the Impact DC Asthma Program at Children’s National Hospital Dr. Stephen Teach says that when they analyzed their patients at IMPACT DC Asthma Clinic, they saw very clear gaps east of the Anacostia River as well as in the eastern end of Capitol Hill. In these neighborhoods, many more patients had to rely on emergency room visits rather than a primary care doctor to manage their asthma flare-ups.

Tips to alleviate symptoms
In addition to more systemic changes, however, there are a variety of strategies that doctors and allergy sufferers agree most people can use to manage their allergies at home — and if you have access, with the support of a doctor.
Prevention starts every day when you walk in the door. Any allergy-sufferer should change their clothes as soon as they get inside (your clothes are pollen magnets!) and then immediately shower and wash your hair to clear off anything you might have carried inside. You should also frequently change your pillowcase, which can also carry a build-up of allergens. Air purifiers can also help clear the air in your house and checking the pollen count before you go outside can help you make decisions about prevention. Finally, getting an allergy test like Chalabi did can help you better understand exactly what allergies you’re contending with, and whether more intensive treatments might be a good fit for you.
“At least now I can see the path I’m going to,” Chalabi says. “And it’s good to know that once you’ve committed to a treatment, it’s like you’re getting something in return.”
This article is part of Health Hub, DCist/WAMU’s weekly segment on health in the D.C. region. Tune in to WAMU 88.5 every Tuesday or on the NPR One app for a conversation with reporters and newsmakers about local health news.
 Aja Drain
Aja Drain