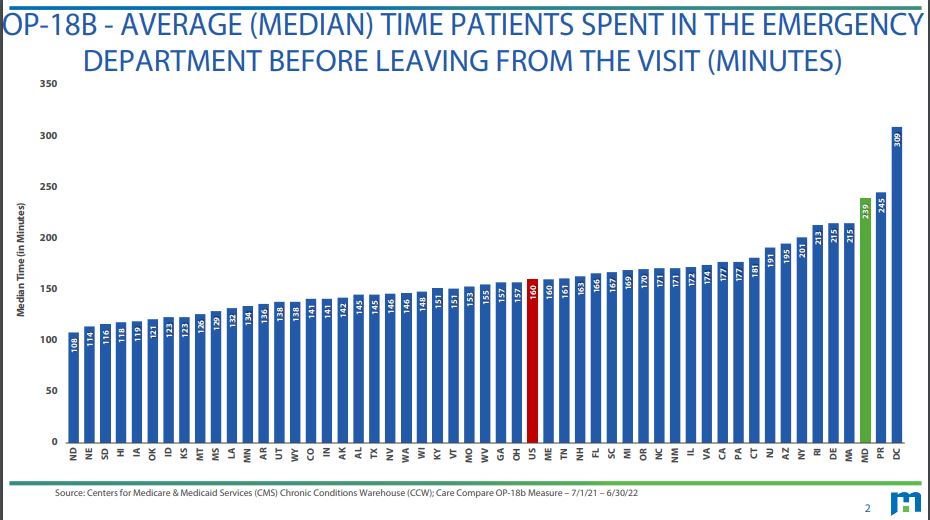
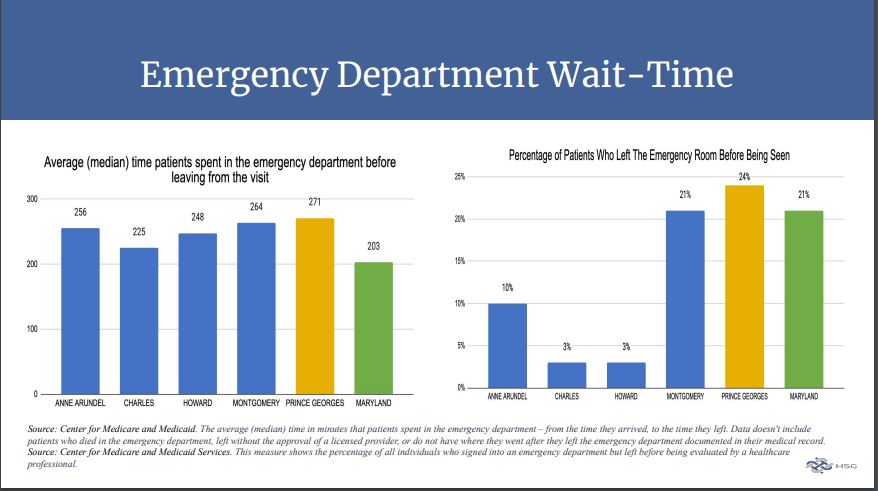
Maryland has some of the longest emergency room wait times in the country, according to the Centers for Medicare & Medicaid Services (CMS) Chronic Conditions Warehouse (CCW), with those in Prince George’s County near the top of the list. The Prince George’s County Council Board of Health met yesterday to hear from health care consultants, providers, and health worker advocates on the issue, as well as to discuss possible solutions.
In Maryland, the average time patients spend in the emergency department is nearly 4 hours compared to the U.S. average of 2.5 hours, according to data presented by the Maryland Hospital Association. And both Montgomery and Prince George’s Counties have patients waiting for around 4.5 hours, according to data from the Center for Medicare and Medicaid.
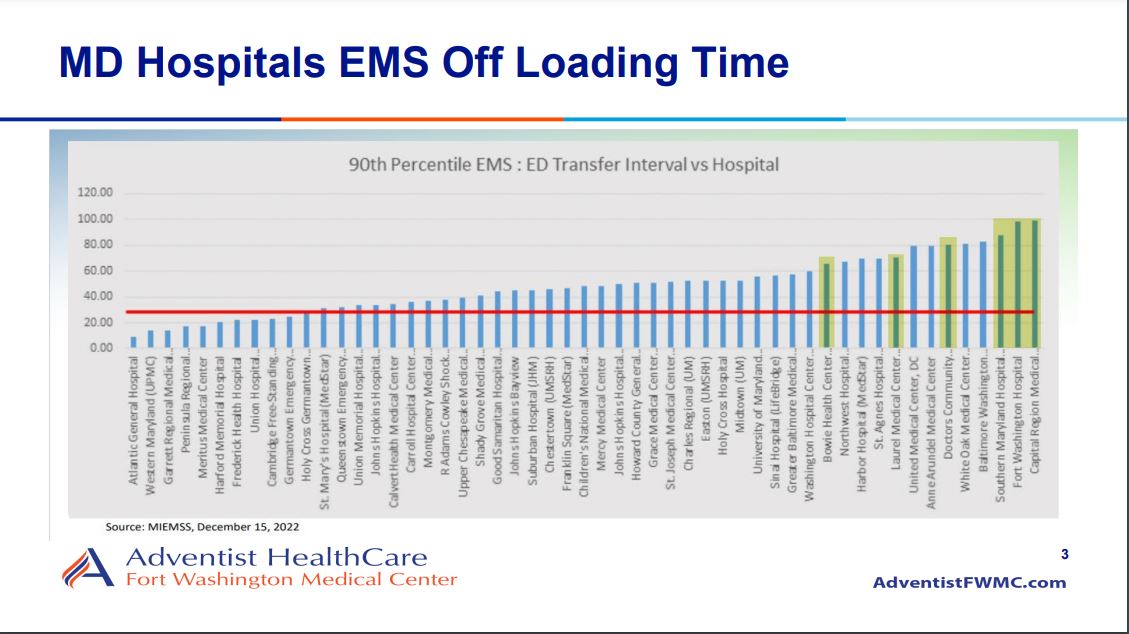
“When it first began in Prince George’s County, there would be occasional times where we had to wait an hour for a patient bed to become available,” said the Vice President of the Prince George’s County Professional Firefighters and Paramedics Association, Grant Walker. “It’s a regular occurrence for our ambulances to wait 2 to 3 hours with a patient in the emergency department, and in some extreme circumstances, [fire and EMS] crews have waited almost an entire 24-hour shift to be relieved.”
Although all of Maryland is struggling with emergency wait times, Prince George’s County suffering the most represents an equity issue that has been present for years. Over 59% of Prince George’s County residents identify as Black, and 21.2% identify as Hispanic, according to the 2020 U.S. Census. But within this minority-majority community, health care access has historically been a struggle in comparison to other counties in Maryland.
There are four hospitals and two free-standing clinics in Prince George’s County; Adventist Healthcare Fort Washington Medical Center, Luminis Health/Doctor’s Community Medical Center, MedStar Southern Maryland Hospital Center, and the University of Maryland Capital Region Medical Center. They are all being impacted by long wait times – with UM Capital Region having some of the worst, according to complaints from residents.
“We did put out a notice for the community to get back to us on their experiences in emergency rooms, and we did get quite a few submissions,” said Councilmember Wala Blegay. “I would say about 70% of the submissions were from Capital Region.”
Hospital executives presented data to the council showing a multitude of intersecting factors that have created and exacerbated these long emergency room wait times.
Staffing shortages are a major issue highlighted across the county – and across the region – particularly for nursing and support staff.
Hospitals were urged to incorporate strategies to ensure worker retention, including improving wages and increasing workforce supply by Lakisa Blocker, a scientist and consultant hired by the Prince George’s County Council Board of Health.
“Workforce shortages have become severe enough that organizations have made them a main focus area in their mid to long-range strategic planning efforts,” Blocker said.
UM Capital Region has lost both ER physicians and nurses, according to Senior Vice President and Chief Nursing Officer of UM Capital Region Health Joel Sandler.
“We have a large number of vacancies, especially in the emergency room, which we have to backfill with very expensive agency and travel nurses, which obviously impacts the financial standing of the hospital,” Sandler said. “We do have our collective bargaining agreement that dictates our staffing ratios, which then forces us to close beds in the emergency room, thus increasing wait times.”
The hospitals are still facing capacity issues within their emergency departments. The University of Maryland Capital Region Medical Center has a 235-bed allotment, but a state health care commission under the Hogan administration decreased that number. There’s a lack of primary care and specialist providers in the county, also creating a burden on emergency rooms.
“When we compare ourselves to Montgomery County, which has about a similar size of the population…we’re about at 20 to 25% of their number of providers per 100,000 on almost every specialty, including primary care, and that is one of the reasons as to why we’re seeing more people coming into the emergency room because they don’t have other choices,” President of Adventist Healthcare Eunmee Shim said in the meeting.
The lack of primary care providers also means that patients with less emergent needs may be using their emergency care to address non-emergent issues – an access problem common across the U.S and could be further exacerbated by hundreds of thousands losing Medicaid.
The county also has a specific demand for behavioral health needs in emergency room departments.
“Behavioral health is becoming one of the biggest concerns in our community, especially as we see our crime rising and seeing that a lot of it is connected with behavioral health and mental health issues,” Blegay said.
Blocker proposed collaborations with sheriff departments, health departments, and county courts to create plans for mental health crisis intervention.
Hospital executives highlighted strategies they are implementing in an attempt to resolve the ER wait times overall. To improve nurse staffing, Adventist Healthcare highlighted its programs dedicated to recruiting international nurses, training immigrants, and educating high schoolers about health career opportunities. MedStar Health has invested in a $41 million emergency department with a dedicated behavioral health space, expanded telehealth for patients, and implemented a transitional care program for a nurse practitioner to follow up with a patient post-discharge to reduce readmissions. UM Capital Region has opened a new Laurel medical center, held nursing town halls, and have executives take rounds to assess workflow in emergency departments.
The state has also developed the Emergency Department Dramatic Improvement Effort (EDDIE) Project, which is dedicated to using public reporting of emergency department performance to improve wait times.
But despite those ongoing measures, executives called on support from the council to increase education in the county and legislation to help enhance and add more medical facilities and support preventative health in the county. But in closing to the four-hour meeting, emergency responders still had concerns.
“When we talk about increasing beds and adding additional facilities, it’s less exciting and more concerning for us when we look at facilities who are mismanaged and aren’t running efficiently now,” Jibran Eubanks, a representative of the SEIU 1199 United Health Workers East. “We heard a lot about retention and recruitment and investing in the workforce, but none of that investing included wages.”
 Aja Drain
Aja Drain