This story was last updated on Oct. 14 at 5:15 p.m.
Cooler weather isn’t the only thing that’s arrived in the D.C. region in the past two weeks — so has an uptick in coronavirus cases.
D.C. and Maryland have both seen increases in their cases per 100,000 metrics since the end of September (Sept. 30 and Sept. 26, respectively). In D.C., the 7-day moving average of the case rate jumped from 5.12 at the end of September to 9.46 today.
In Maryland, the same metric went from 7.63 to 9.61 over roughly the same period. At the county level, Montgomery County’s trend roughly tracks the whole state, though its case rate has mostly stayed lower. Prince George’s County’s case rate is higher than the state, but it has been trending slightly downward since the beginning of the month.
The metrics are still significantly better than they were in the spring, and experts say it’s still too soon to suggest the uptick is an indication of a second surge of cases in the region. But the trend is still worth monitoring, says Dr. David Marcozzi, an Associate Professor of Emergency Medicine at the University of Maryland School of Medicine and the leader of the University of Maryland Medical System’s COVID-19 response.
“We’re starting to see a change in the slope of the line with regard to case positivity,” says Marcozzi. “And the question is, will that result in hospitalizations? We’re watching that closely.”
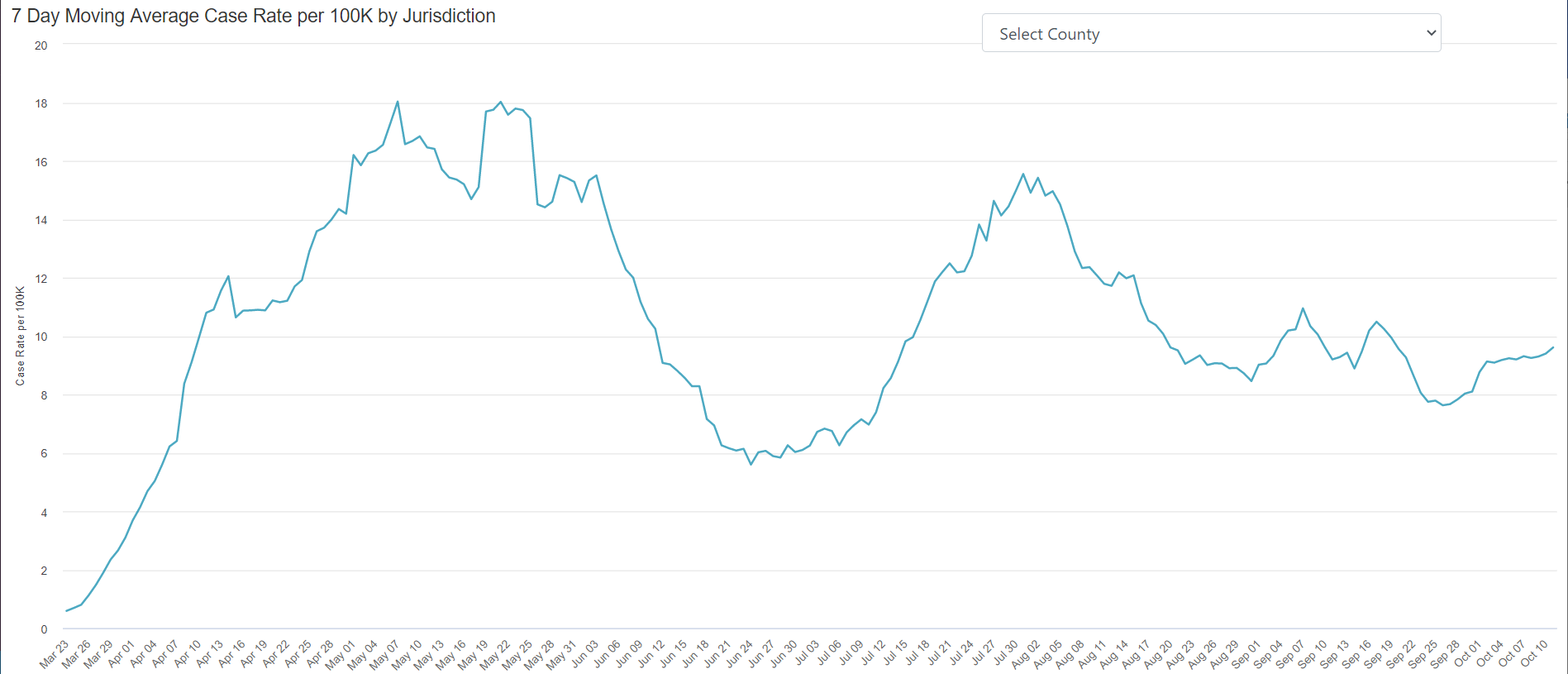
Today, Maryland also passed a sad milestone: more than 4,000 Marylanders are now confirmed or suspected to have died from COVID-19.
In Virginia, cases have shown a less steady trend since the end of September, though they have been increasing since Oct. 7, including in the northern part of the state.
It’s hard to know exactly what’s behind the upward trends, but experts have a few ideas. One possible factor is a lagging result from travel over Labor Day weekend.
“Once you travel to one place and then come back, you may not see that uptick because you may spread it to someone else and then someone else, and then that person gets hospitalized,” Marcozzi says. “You may not see that hospitalization impact for potentially weeks to months later as it moves between individuals.”
Dr. Cliff Mitchell, who directs the Maryland Department of Health’s COVID-19 response in business, higher education and correctional settings, says the state has been monitoring higher resident mobility since Maryland moved into Phase 3 of its reopening plan. That trend is to be expected, he says.
“It doesn’t come as a surprise to anybody that with moving into stage three of the Governor’s Roadmap to Recovery, we have seen some increases in areas around the state,” he says.
Mitchell and Marcozzi note that there’s been an increase in viral spread among younger people and in informal settings like birthday parties, bars, or college dorms. Marcozzi has one message for people engaging in those higher-risk activities: “Those folks need to know that we’re all in this together, and the better they do with limiting their spread of this virus [that] will benefit us all,” he says.
Another factor at play is general fatigue with complying with social distancing measures and mask-wearing, Marcozzi says. He recognizes the significant mental health challenges at play, but ultimately, there’s nothing else to do but keep going.
“We need to just continue our motivation so that we don’t have that struggle and that breakdown, and therefore the virus spreading between us as a result of that fatigue,” he says.
Mitchell says he’s concerned about people getting lax about social distancing, too.
“While we’ve been trying to encourage people as much as possible to continue to use social distancing and face covering, I think that we have seen signs that some of that is not as effective as it was previously,” he says.
The D.C. region is currently home to a very high-profile coronavirus outbreak at the White House. It’s too early to tell, Marcozzi says, whether the cluster of cases associated with the Trump Administration could influence a broader regional uptick in cases. D.C. only counts current District residents towards its case numbers (meaning that President Donald Trump, for instance, who is not officially a D.C. resident, doesn’t count in the city’s accounting). But city health officials believe the White House outbreak could be contributing to recent higher demand for coronavirus testing, and DC Health set up a one-day public testing site next to the White House to encourage staff to get tested.
The upward trend in D.C. and Maryland case rates comes as the region confronts a slew of new factors that could impact the coronavirus response: the arrival of cold and flu season, colder temperatures which could drive people to socialize indoors where transmission is higher, and officials’ hopes to begin a partial reopening of public schools.
Given all of that, Marcozzi says it’s important to scrutinize the case numbers these days, even if they situation in the region is still, on the whole, in a good place.
“We all know that as we move inside, as things get colder and we all get tired of wearing masks and physically distancing, that this virus will spread more,” he says. “And it is something we need to be aware of, because the risks of the fall and winter may actually be worse than the spring.”
Mitchell agrees that even small upticks in cases now can be significant. The summer was the region’s chance to get the virus under control, before the change in seasons brings new challenges to preventing skyrocketing growth in cases.
“We’ve had sort of the best possible shot at reducing COVID [during the summer] due to the fact that people could spend a lot of time outside,” he says. “Even small increases can be problematic because at some point or the other, you reach the point where it becomes very hard to bring things back into control.”
This story has been updated to add comments from Dr. Cliff Mitchell, and to reflect that Dr. Marcozzi is affiliated with the University of Maryland School of Medicine.
 Margaret Barthel
Margaret Barthel



