Update 1/11: D.C. Mayor Bowser declared a limited public health emergency after hospitals requested additional support and flexibility in order to respond to an unprecedented COVID-19 surge. The emergency is effective immediately and lasts until Jan. 26. The governors of Maryland and Virginia also declared limited emergencies to help overwhelmed local hospitals.
“Given the ongoing impacts of COVID-19, the vast rise in new cases and visits to the emergency rooms, continuing deaths from COVID-19, and staffing shortages at medical facilities due in part to staff being out with COVID-19, the District must declare a limited public health emergency to appropriately protect public health,” the order says.
Hospitals have the physical capacity, including enough beds, to treat patients but struggle due to staffing shortages, according to the order. Some hospitals have 25% of staff out due to COVID-19-related leave. Emergency rooms, in particular, are overwhelmed with an influx of patients.
The order empowers DC Health Director Dr. LaQuandra Nesbitt, or a designee, to issue administrative orders. It is not immediately clear what recommendations from the DC Hospital Association that DC Health is implementing. Bowser’s press secretary Susana Castillo tells DCist/WAMU that they expect to publish orders “in the coming days.”
Original: A significant number of people are visiting D.C. hospitals just to get tested for COVID-19 or to treat mild coronavirus cases, adding additional stress on overworked health care workers, a D.C. health official said on Thursday. The health care system is already so strained that the D.C. Hospital Association is recommending that D.C. Mayor Muriel Bowser declare a new public health emergency in order to enable additional resources and flexibilities.
At a press conference Thursday, the Mayor and DC Health senior deputy Patrick Ashley encouraged residents to stay home if they test positive and are not experiencing life-threating symptoms like shortness of breath. Residents should get tested at a public library or firehouse, and officials advised getting a booster shot if eligible. Kids who are between the ages 12 to 15 who received the Pfizer vaccine on or before Aug. 6 just became eligible to get boosted, and can now get the extra shot at government-run sites or private clinics. D.C. residents can also call 855-363-0333 to book an appointment to get vaccinated at home.
“There are a lot of free opportunities in the community, so please take advantage of those,” said Mayor Muriel Bowser during the press conference.
“Emergency rooms are for emergencies,” added Ashley.
As of Jan. 5, the D.C. hospital system was at 84% capacity, said Ashley. He also said hospitals are seeing a “significant” volume of COVID-19 patients, however it’s unclear how many of the 624 patients landed in the hospital because of COVID-19 as opposed to another service but tested positive during screening.
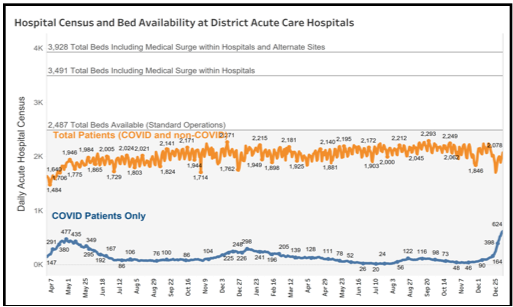
While vaccination has helped reduce the number of people who get seriously ill from COVID-19, local hospitals are still strained. On Jan. 5, the D.C. Hospital Association wrote the Deputy Mayor for Health and Human Services, requesting the additional resources and flexibility afforded earlier in the pandemic to address the outsized needs.
“The impact on health care is currently greater than at any time in the pandemic given the significant community spread and resulting increase in the number of patients requiring admission,” writes DCHA President and CEO Jacqueline D. Bowens. “The impact to health professionals and support personnel who are testing positive for COVID, due to this significant community spread, is also a major factor. This strain is felt throughout the health care continuum.”
The D.C. Hospital Association recommended the mayor declare a new public health emergency that would authorize hospitals to use “Crisis Standards of Care,” which allows decision-making based on what produces the best outcome for a group of patients rather than an individual one. Hospitals would be able to implement “surge capacity” strategies like triage and risk communication. The association that represents 13 local hospitals also wants to be empowered to address the staffing shortages by hiring new health professional graduates, under supervision, authorizing inactive practitioners, and expanding the scope of practice for some providers when necessary.
Notably, the association advised against a blanket prohibition on “non-urgent but medically necessary procedures/surgeries.” “Curbing non-urgent but medically necessary procedures/surgeries could lead to unnecessary pain, as well as increased morbidity and mortality in patients. As you know delaying care during the first surge negatively impacted patient care and hospitals and providers continue to manage the catch-up on the delayed care from the pandemic,” writes Bowens.
To help address the issue of people showing up to the hospital just for COVID-19 testing, the D.C. Hospital Association is asking the District to set up additional testing sites next to hospitals and ambulatory care centers. Maryland Gov. Larry Hogan just signed an executive order along those lines, instructing the National Guard to open 20 testing sites outside of hospitals in the hopes of diverting people away from overwhelmed emergency rooms. Some are already open.
The D.C. Hospital Association also thanked the Bowser administration for the support offered so far. In late December, the administration announced a $15-million grant for hospitals to address staffing needs. At the time, Ashley said one in four hospital workers were out due to COVID-19 isolation or quarantine.
During Thursday’s press conference, Ashley said the Bowser administration has not made any decisions “about adding other liability protections or crisis standards of care at this time.”
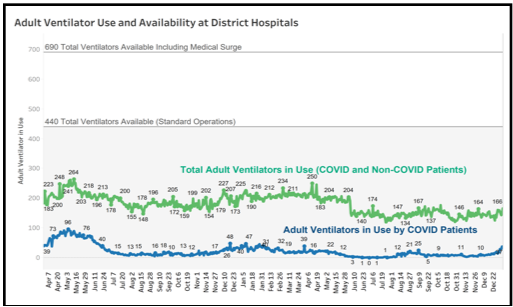
According to DC Health’s key metrics, hospitalizations amount to 4.4% of cases, based on a 14-day rolling average, suggesting someone’s risk of hospitalization is relatively low. The ICU beds are not being filled up with patients who are fully vaccinated, said Ashley.
“Taking care of 624 COVID patients in the hospital does put additional stress on the hospital,” added Ashley. “Our hospitals are doing well. We are in daily communication with them but we are trying to make sure we are not adding any additional burden to them.”
“There’s always concern about capacity,” Ashley continued.
This story was updated to change a photo caption stating an incorrect total of COVID deaths.
 Amanda Michelle Gomez
Amanda Michelle Gomez



