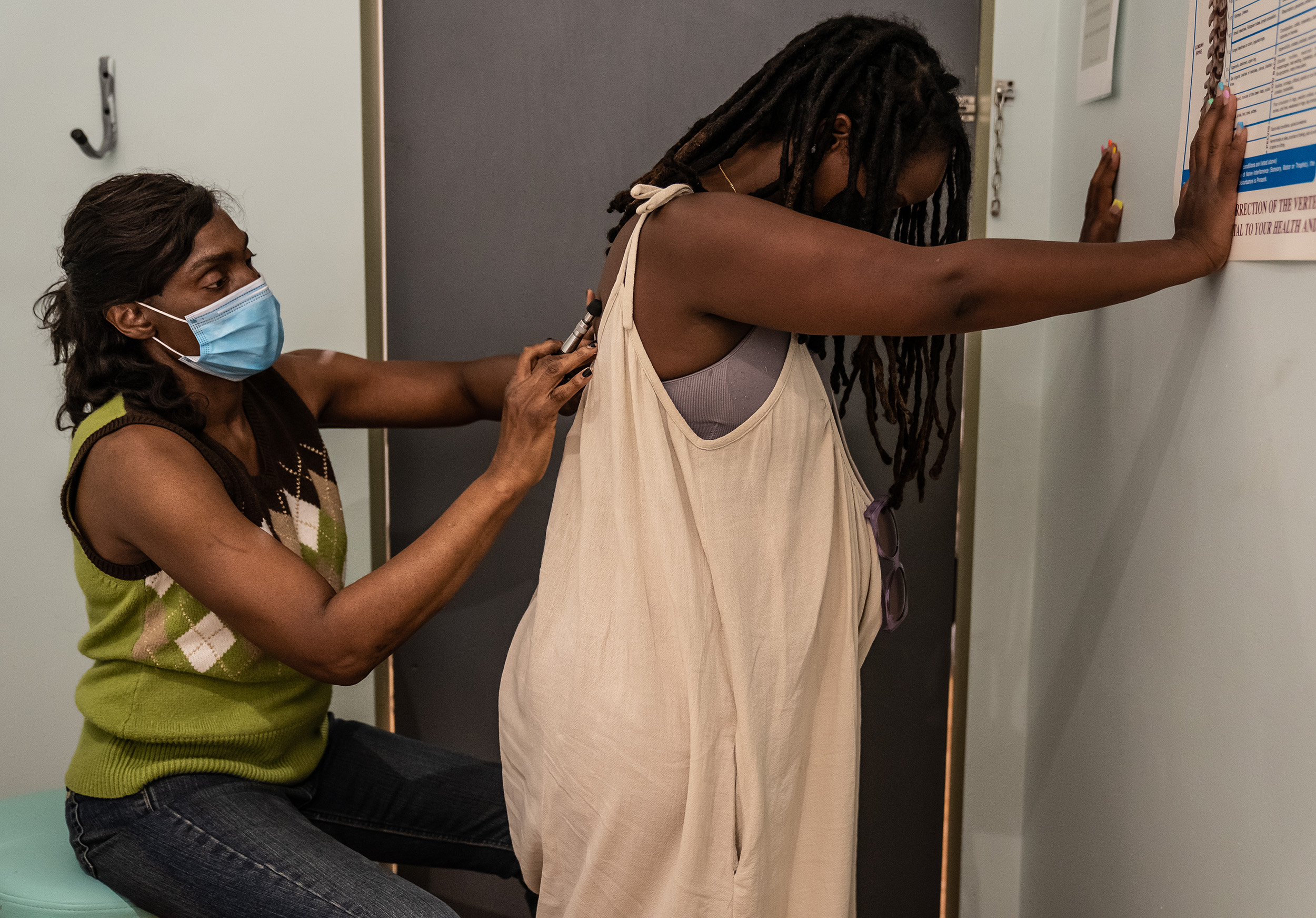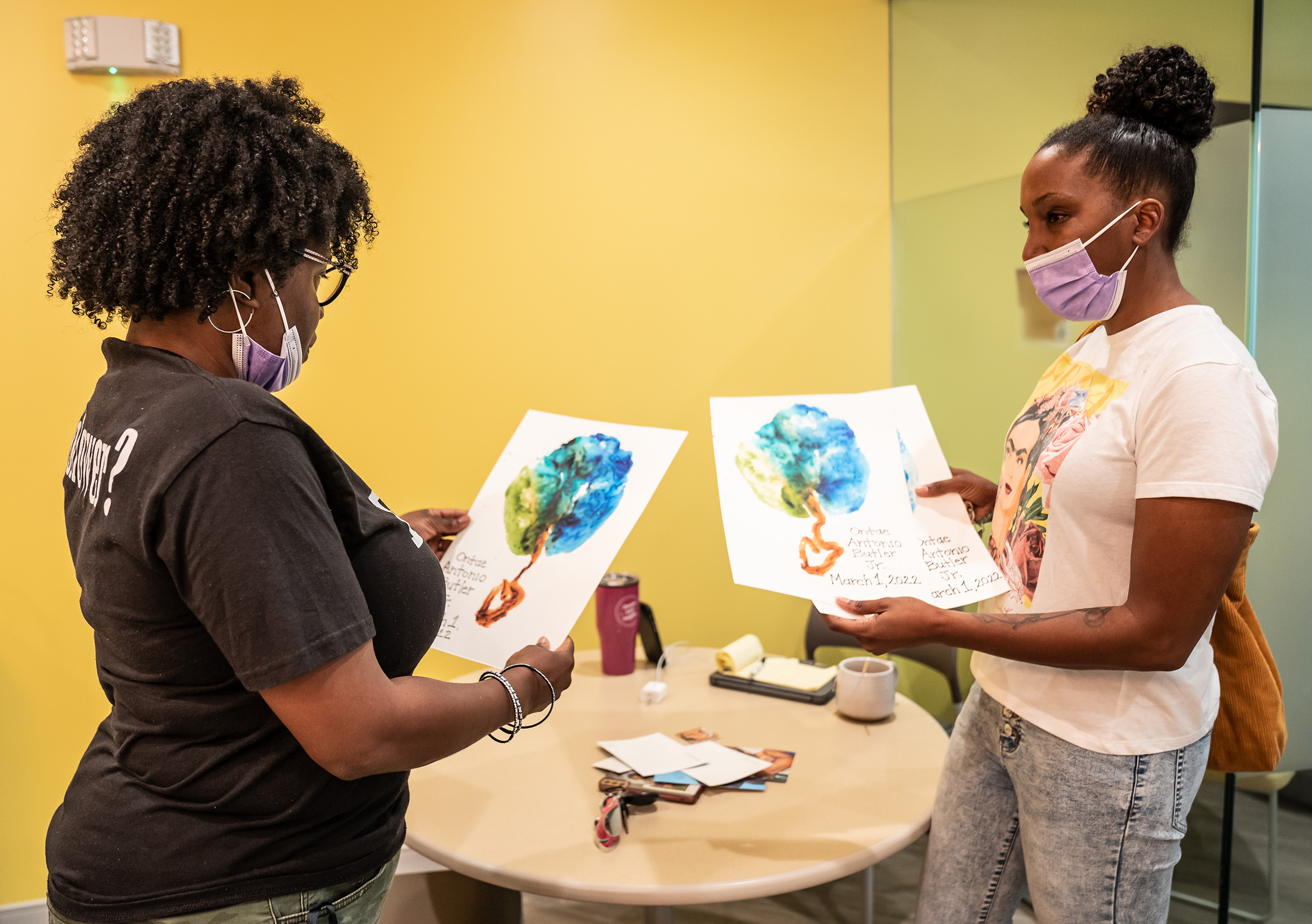Tsedaye Makonnen is reclining on her couch, in her home in Northeast D.C. She’s 33 weeks pregnant, and she’s surrounded by three other Black women — a midwife and two trainees — who are performing a routine prenatal exam.
The women take her blood pressure, measure her belly, and check on her overall well-being. One of them balances an iPhone so that Makonnen’s partner can join the appointment remotely. They talk about how to prepare for an at-home birth, discuss a recommendation for a culturally competent pediatrician, suggest some exercises to help adjust the position of the fetus for an easier birth, and go over Makonnen’s overall nutrition and wellness. They also laugh and joke: the group dissolves into laughter when Makonnen, who usually eats vegetarian, admits she’s been craving ribs.
Makonnen chose at-home care for the birth of her son, who is now in elementary school, and for this second pregnancy, too. Home, she says, “is comfortable.” And so are the people she’s with.
“I intentionally wanted to work with Black practitioners, because that’s who I feel the safest with,” she says. “Culturally, there’s just an understanding and a level of support that they can provide that other health practitioners can’t.”

It’s supposed to feel like that, says midwife Aza Nedhari, who is overseeing Makonnen’s care.
“Every visit we’re building rapport, checking in on how the mother’s doing, how she’s feeling. There’s lots of laughs and hugs,” she says.
Both women know what the alternatives feel like, too. Makonnen has worked alongside Nedhari as a doula, advocating for Black patients in traditional medical settings, where they often face racist assumptions, microaggressions, and other barriers to effective care.
Makonnen traces those dynamics back to the history of racism and white supremacy in the field of gynecology. Early practitioners, including the so-called “father of gynecology,” performed forced experiments on enslaved Black women that launched the field in the first place.
“I think that the whole thing needs to be dismantled,” Makonnen says. “Power needs to be given back to the midwifery community.”

Taking some of that power back for Black birth workers in D.C. is Nedhari’s life work. Outside of her private practice, Blue Sage Midwifery, she’s the co-founder and executive director of Mamatoto Village, a Black birth worker collective that offers pre and postnatal wraparound care for primarily Black and immigrant women residing in Wards 7 and 8.
Mamatoto Village is tackling a major problem in D.C.: bad outcomes for Black pregnant people, including preterm births, lower birth weight babies, and even death in comparison with their non-Black counterparts.
Between 2014 and 2018, D.C. lost three dozen residents within one year of their pregnancy due to related causes, according to a report from a District committee tasked with reviewing maternal deaths in D.C. (Nedhari is one of the co-chairs). 93% of them were Black. 70% had lived in Wards 7 and 8.
Experts say those losses are rooted in structural racism: the lack of resources in predominantly Black neighborhoods, the challenge of getting to prenatal appointments across the city, the biased way the medical community can treat Black patients.
“There’s only three grocery stores east of the river,” Nedhari points out. “People have to beg the council, they have to beg their city — that they pay taxes to — to provide basic necessities for them. And so to me, the maternal health issue is just one piece of a multitude of issues that are happening with people in this city.”
Mamatoto Village serves some of the most at-risk pregnant patients in the District. In general, about 40% of their patients are housing insecure, 80% live below the poverty line, and 80% are food insecure.
Last year, 88% of their patients were Black, and 61% lived in Wards 7 and 8. All of them were eligible for Medicaid.
Statistically, people are much more likely to have negative pregnancy outcomes in D.C., or even to die. But that’s not happening for Mamatoto Village’s clients. Since the organization started serving families in 2013, they have not lost a patient due to pregnancy-related causes. In 2021, they took care of 144 patients, 70% of whom had vaginal deliveries. 80% avoided the neonatal intensive care unit. 80% also had babies of normal birth weight and the same percentage began breastfeeding.
“We’re not the prescription, but we are one prescription for addressing that problem,” Nedhari says.
That prescription is rooted in a deep knowledge of the community it serves, a celebration of Blackness, and a relentless commitment to providing care and advocacy for pregnant patients and their families.
Mamatoto Village cares for patients throughout pregnancy, during birth, and afterwards. Staff perform home visits to check in with pregnant patients and accompany them to traditional medical appointments. They offer culturally-competent midwifery — plus counseling, parent education, support for breastfeeding, and a variety of wellness services geared to helping patients eat healthy and exercise.

“Our model of collective care provides the community you need to thrive; the resources to birth and parent on your own terms, and the pathways leading to personal transformation,” the Mamatoto website says.
Mamatoto Village accepts insurance from a variety of Medicaid managed care organizations. The nonprofit also reserves space each quarter for people who don’t have the insurance they accept, or who are uninsured.
Mamatoto’s staff is Black, and many are from the community they serve. They are perhaps one of the biggest testaments to Mamatoto’s success: several have come in for care and chosen to stay on as employees.
“It was all consuming. It was amazing. And then from there I was like, ‘Oh, I need to be part of this,’” says Jazzmin Shakir, the education specialist at Mamatoto Village, who has also served as a Mamatoto-trained perinatal community health worker — “a cross between a doula and a social worker,” as she defines the role. Training more Black birth workers is a key goal of the nonprofit.
Shakir came to Mamatoto after she put out a desperate call on Facebook for help in finding support during her pregnancy in 2015. A friend’s recommendation and a tearful but relieved phone call later and she was officially a client.
During her pregnancy, Mamatoto staff helped Shakir understand what was happening to her body, and helped her know what questions to ask of medical providers.
“Just learning little tiny things will allow you to advocate for yourself, will allow you to really take on this whole pregnancy and this life changing experience,” she says.
Other Mamatoto staff have first-hand experiences of pregnancy and birth that were far less supportive.
“Just not having the tools, not having the support really just sent me down a path of just trauma all the way through to having [my first daughter],” says Dionne McDonald, who has been on staff since 2014.
Her experience with her first pregnancy made McDonald start asking questions and researching about Black birth experiences. A friend eventually suggested she take Mamatoto’s training course for perinatal community health workers, and she found her calling in the work. She estimates she’s supported hundreds of Black families in pregnancy and birth.
“I’ve seen every part of the life cycle,” she says. “I’ve walked the path with so many families in this city, and in that I’ve healed from my trauma too.”
Now, McDonald helps Mamatoto Village with intake — bringing families who’ve been referred by a medical provider into the Mamatoto community and helping them learn what’s available to them.
“In our society, Black women are the most unprotected,” she says. “That’s my life mission: to give a different kind of energy to my sisters.”
Soon, Mamatoto Village will be able to support more families. In June, they opened a brand new clinic on Sheriff Rd Northeast.
In the new center, they plan to hold group yoga classes, social events for soon-to-be parents, and other activities to help patients develop and deepen their sources of community support. They’ll be able to see patients in exam rooms for the first time, though home visits will also continue.
The new clinic doubles the size of the nonprofit’s previous space, and includes exam rooms, a full kitchen, a community room and office space. And in keeping with Mamatoto’s care model, the whole place is meant to welcome the surrounding community in.
“It was really important for this space to feel like a home when you walk in,” Nedhari says.

The clinic rooms are painted in restful shades of blue and purple and the lights can dim to anyone’s preference. Images of Black people at every stage of motherhood hang on the walls, and children’s books by Black authors are scattered around. None of that is an accident, says Nedhari.
“That cultural reflexivity is really, really important, that people here feel honored right about who they are as a Black person, that they don’t feel like being Black is associated with oppression,” she says. “We want them to feel uplifted. We want them to feel proud of who they are in the history and lineage that they are a part of.”
That sensibility informed the entire process of acquiring the property and designing the clinic, from start to finish. Nedhari and her team worked with a Black-owned real estate company to acquire the property. The sister of the clinic’s Director Of Operations, Briana Green, designed the interiors of the space.

Now that it’s operational, Nedhari and her team plan to hold healthy cooking classes in the kitchen, where they’ve also started a milk dispensary for community members who can’t breastfeed. There’s a big space for yoga and other classes and community meetings.
Opening the new clinic itself is a big step, but Nedhari already has her eye on expanding Mamatoto Village’s footprint even further.
“My biggest hope and aspiration is that we will have this block of a village, [and] that people walk the block and they’re like, ‘That’s Mamatoto. I know that that’s the space for me,’” she says.
This post has been updated to clarify that Jazzmin Shakirr’s title is education specialist and that Briana Green’s sister designed the clinic’s new space.
 Margaret Barthel
Margaret Barthel Dee Dwyer
Dee Dwyer Amanda Michelle Gomez
Amanda Michelle Gomez